What are autoimmune disorders? An autoimmune disease occurs when your immune system mistakenly attacks your body rather than protecting it. Over 100 autoimmune disorders have been identified. Lupus, rheumatoid arthritis, Crohn's disease, and ulcerative colitis are some of the most common. This article will cover the conventional medical treatment, as well as the natural medicine treatment.

 Autoimmune disease treatment is certainly possible with natural medicine. This article will continue with auto-immune conditions but offer some solutions as to the prevention and treatment of various auto-immune conditions. In Autoimmune Disease you can read about what auto immune disease actually is. Did you know that being overweight and, in particular, obese, is the enemy of disease recovery?
Autoimmune disease treatment is certainly possible with natural medicine. This article will continue with auto-immune conditions but offer some solutions as to the prevention and treatment of various auto-immune conditions. In Autoimmune Disease you can read about what auto immune disease actually is. Did you know that being overweight and, in particular, obese, is the enemy of disease recovery?
First, I’d like to discuss inflammation and the reasons you want to conquer it, it is one of the most important “drivers” behind most chronic disease, then we discuss the medical treatment, and finally the natural treatment of autoimmune disease. I’ll be talking more about foods than dietary supplements. You are best to work with your practitioner with supplements.
Autoimmune disorders such as multiple sclerosis, rheumatoid arthritis, and Type 1 diabetes are among the leading causes of death among women under age 65, according to a study in the US Journal of Public Health (Sept. 2000) They do not classify autoimmune diseases in the same way as other diseases such as heart disease, diabetes or cancer. Their high mortality rates have gone unrecognised because of this.
Most autoimmune disorders are not on “the list”, prepared by the statistics that doctors use when recording cause of death. For example, American researchers examined national mortality data for 1995 from the Center for Disease Control and Prevention (CDC), looking for mention of 24 different autoimmune disorders, and found that, when grouped together, these disorders accounted for much of the deaths, putting it among the top 10 causes of death in women.
Who would have thought that autoimmune disease is one of the top ten killers of women. We have such a major group of diseases which cause lots of health problems, particularly in women, which account for such a high number of death and disability, yet we have no real concrete idea of the cause. Let’s first look at inflammation, the driving force behind autoimmune disease, and if it is possible to turn down the inflammation.
 Many auto-immune conditions have a component of inflammation, and this can spell pain for many with conditions such as rheumatoid arthritis, ankylosing spondylitis and many other manifestations of auto-immunity. What we want is to switch off this pain signal, and we can help the body achieve this in several ways. The aim is with any autoimmune treatment plan, regardless if it is conventional medical and natural treatment, is to reducing inflammation by correcting the biochemical pathways involving the body’s faulty immune system. It makes the most sense (to me) with auto-immunity to regenerate the very system, which reduces the body’s inflammation naturally, the adrenal glands.
Many auto-immune conditions have a component of inflammation, and this can spell pain for many with conditions such as rheumatoid arthritis, ankylosing spondylitis and many other manifestations of auto-immunity. What we want is to switch off this pain signal, and we can help the body achieve this in several ways. The aim is with any autoimmune treatment plan, regardless if it is conventional medical and natural treatment, is to reducing inflammation by correcting the biochemical pathways involving the body’s faulty immune system. It makes the most sense (to me) with auto-immunity to regenerate the very system, which reduces the body’s inflammation naturally, the adrenal glands.
Many people accept their lot as far as chronic pain and auto-immunity and powerful drugs are concerned. This is partly due that the primary focus of medical treatment is to suppress the symptoms, particularly in reducing the pain. With pain control, the case is virtually closed, and they keep the patient on combinations of various pills, including anti-inflammatory drugs. They will recommend this treatment “for life”.
Prolonged dosages of pain-killing drugs and anti-inflammatory preparations are not the solution, simply because their long-term side effects are so severe on the human body.
A study from 2010 about natural medicines and inflammation: “For centuries, natural anti-inflammatory compounds have been used to mediate the inflammatory process and often with fewer side effects. We have briefly reviewed several of the most commonly used plant- and animal-derived natural compounds that may possess similar effectiveness in treating the inflammatory reaction seen in both chronic and sub-acute pain syndromes encountered in a typical practice.”
 Some Get Addicted To Pain Medications
Some Get Addicted To Pain MedicationsThe stronger reliance on pain relief, the bigger the problem when one day you reduce dosages or decide to come off these drugs. I had a patient once who was considerably overweight with a bad back. But instead of losing weight through sensible eating and exercising, his lifestyle remained unchanged. He remained on increasingly powerful painkillers, including morphine. His condition got worse, he became hooked on pain relief. Such addictions kill far too many people. It’s truly sad. Your naturopath or natural health care professional can usually offer you non-pharmaceutical drug ways to decrease inflammation and show you how natural medicine can be of benefit. Acupuncture has been of benefit to several of our auto-immune patients by decreasing inflammation, and I refer a patient to a skilled acupuncturist is many cases.
 Conventional treatment involves monitoring the condition, preventing flares and treating the symptoms with drugs when they occur. Commonly, anti-inflammatory drugs form the mainstay of treatment, along with steroids for the flare-ups.
Conventional treatment involves monitoring the condition, preventing flares and treating the symptoms with drugs when they occur. Commonly, anti-inflammatory drugs form the mainstay of treatment, along with steroids for the flare-ups. They commonly use these drugs in the treatment of moderate-to-severe cases and work by suppressing inflammation. Doctors can prescribe them as tablets or as a cream, or injection. Examples are prednisone, hydrocortisone and dexamethasone. They work, and can help with the pain quickly, but you rapidly gain dependence on them and some find it very hard to reduce your dosage. Adverse effects are related to dose and duration of treatment, and can increase steeply once the dosage exceeds 7.5 mg of prednisone daily.
They commonly use these drugs in the treatment of moderate-to-severe cases and work by suppressing inflammation. Doctors can prescribe them as tablets or as a cream, or injection. Examples are prednisone, hydrocortisone and dexamethasone. They work, and can help with the pain quickly, but you rapidly gain dependence on them and some find it very hard to reduce your dosage. Adverse effects are related to dose and duration of treatment, and can increase steeply once the dosage exceeds 7.5 mg of prednisone daily.
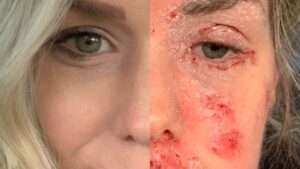 Be Very Careful With Steroids And Your Skin!
Be Very Careful With Steroids And Your Skin!Adverse effects include osteoporosis,Increased susceptibility to infection, cataracts, weight gain, increased appetite, bruising, hirsutism (facial hair), flushing, acne and redistribution of body fat, creating the typical moon face and “buffalo hump” on the back. Your adrenal glands may suffer from this immune suppression on steroids, and a good recommendation is to support the adrenal glands with herbs and nutrients whilst you are taking steroids. It can make all the difference. This is my experience after working with many patients who were taking steroids, especially long-term in autoimmune disease conditions.
 These help to “dampen down” the abnormal response of the immune system. Examples of these medications include azothiaprine, methotrexate and cyclophosphamide. Because these drugs are potent and toxic to your body, be sure to only use them for short durations. I would recommend a liver and kidney cleanse after you have finished a course of these drugs to ensure an adequate clearance from the body, but you may avoid them. Talk with your doctor.
These help to “dampen down” the abnormal response of the immune system. Examples of these medications include azothiaprine, methotrexate and cyclophosphamide. Because these drugs are potent and toxic to your body, be sure to only use them for short durations. I would recommend a liver and kidney cleanse after you have finished a course of these drugs to ensure an adequate clearance from the body, but you may avoid them. Talk with your doctor.
They have used immune system-suppressing drugs have recently in autoimmune disease, in dosages high enough to treat cancer or keep the body from rejecting transplanted organs. Early results have been promising, but I fear in this situation that there will be adverse outcomes, just like there have been for other drug-based treatments.
But there are other options besides pharmaceuticals, like physical therapy. For example, physical therapy can help control or stay the effects of diseases like rheumatoid arthritis and multiple sclerosis, which can cause stiffness in the joints or weakness in the muscles.
 High Body Fat Increases Inflammation
High Body Fat Increases InflammationAccording to Dr. Barry Sears, President of the Inflammation Research Foundation, stored fat is a very active source of “silent” inflammation. Therefore, the first line of defence against inflammation should be the reduction of body fat because it produces an excess of the hormone called insulin. As the glycemic (carb) load of the diet increases, your pancreas secretes more insulin. This, in turn, activates a powerful enzyme (Delta 5 desaturase), which produces arachidonic acid (AA). As the level of AA increases in the fat cells, it produces more inflammatory mediators. The result is an increase in systematic inflammation that started with an increase in “silent” inflammation in the fat tissue. Thus, the current obesity epidemic is in reality an epidemic of silent inflammation! This is very relevant information, because our obesity has more than doubled in the past 30 years. Research has shown that being overweight can cause you pain through increased inflammation.
 Here are some of the most important steps you can take, in no particular order. How many of the following 6 points are you currently adhering to? These are the points I would discuss with patients in our clinic in some detail and give information about. If you have active autoimmune disease, then I’d encourage you to follow as many of these points as possible. It will surprise you when you maintain these healthy habits for 6 to 12 months. You’ll require less anti-inflammatory drugs.
Here are some of the most important steps you can take, in no particular order. How many of the following 6 points are you currently adhering to? These are the points I would discuss with patients in our clinic in some detail and give information about. If you have active autoimmune disease, then I’d encourage you to follow as many of these points as possible. It will surprise you when you maintain these healthy habits for 6 to 12 months. You’ll require less anti-inflammatory drugs.
 Anti Inflammatory Diet
Anti Inflammatory Diet The autoimmune diet is an anti-inflammatory diet. There never will be a natural treatment (or drug) which can overcome or negate the effects of a poor diet, inadequate nutrition, lack of exercise, and an unhealthy, stressful lifestyle.
Studies now emerge that point the finger at what we eat, and the global spread of autoimmune disease is being increasingly blamed on western diet
Your diet is one of the most important interventions for autoimmune disease. Other issues that are frequent problems are emotional stresses in your life, and I’ve often seen patients who have had so much stress in their lives, culminating in the eventual breakdown of their immune system. Over all, when you are choosing anti-inflammatory foods to help reduce your inflammation and pain, choose fresh foods instead of heavily processed foods.
Weight loss is not the goal of an anti-inflammatory diet, but it is common for people who follow it to lose weight. Your aim is to stop “chronic silent inflammation” in the body, that occurs when the immune system doesn’t know how to stop working. The theory is that the body’s defences remain switched on, even after the bacteria or viruses that caused an infection are gone. These activated immune cells and hormones then turn on the body itself, damaging tissues. The process keeps ongoing and is so slow that a person doesn’t feel pain or recognise anything is wrong. Supporters say that the damage causes health problems like autoimmune diseases, heart disease, Alzheimer’s disease, and even cancer many years later.
Are you wanting to reduce your inflammation if you currently have an autoimmune disease? Perhaps you want to prevent heart disease, Type 2 diabetes, cancer or another chronic illness from developing or reduce your dependence on pharmaceutical pain killers? An anti-inflammatory diet doesn’t require any unusual or pricey materials, such as powders or supplements, and the bonus is that many of these foods taste great as well.
Natural foods can have powerful anti-inflammatory actions. Flavanols, for example, are anti-inflammatory chemicals found in red wine, grapes, and some berries. Fatty fish like salmon contains omega-3 fatty acids. They have studied these good fats for years and known them to reduce the inflammatory response. Have they have diagnosed you with an autoimmune disease? I recommend anyone in this situation to choose a plate full of vegetables and fruit, as well as lean protein and whole grains, for an anti-inflammatory diet. The following foods are some of the best I know in reducing inflammation and boosting your immune function. Try to add one or all of them to your diet. It may well be one of those turning points in your life, like it has been for the many autoimmune patients I’ve seen in the past.
 Avocado
AvocadoResearch has discovered that the average avocado consumption is one-half fruit, which provides for a nutrient and phytochemical dense food comprising significant levels of: dietary fibre, potassium, magnesium, vitamin A, vitamin C, vitamin E, vitamin K1, folate, vitamin B-6, niacin, pantothenic acid, riboflavin, choline, lutein/zeaxanthin, phytosterols, and monounsaturated rich oil.
Research discovered that 51 adults who were overweight who consumed avocados over a period of 12 weeks were found to have lower levels of the inflammatory markers CRP and interleukin 1 beta (IL-1).
The avocado is likely one of the world’s top super foods. In fact, avocados have such potent anti-inflammatory qualities that eating them may actually compensate for eating other foods that aren’t as healthy. It’s crazy. We have two Hass avocado trees; I planted them in 2012 and today yield many hundreds of fruit each year. Consider growing a tree containing the world’s healthiest fruit. Your neighbours may end up becoming your best friends!
 Berries
BerriesFor lowering inflammatory levels, berries are tiny superfoods that deliver quite the punch. Densely packed blueberries containing dietary fibre, vitamins, and minerals and antioxidants called flavonoids that can help reduce inflammation. They include substances that help regulate your immune system, which can lead to a reduction in chronic inflammation. There are many berries, but the best are blueberries, raspberries, blackberries and strawberries. Anthocyanins are the name of the antioxidants that are found in berries. These chemicals have anti-inflammatory actions, which may lower the risk of disease for individuals who consume them. Studies have shown that they also known berries to increase the amount of natural killer cells (NK cells) your immune system makes, and their presence contributes to the optimal operation of your immune system. A randomised control trial (study 2011) revealed that daily blueberry consumption for 6 weeks increases NK cell counts, and acute ingestion reduces oxidative stress and increases anti-inflammatory cytokines. Can you see why we grow lots of blueberries at our place?
 Broccoli
Broccoli
Studies have found that the nutritional value of broccoli is one of the highest of all leafy green vegetables. It is a member of the cruciferous vegetable family, the same family as cauliflower, kale, cabbage, Brussels sprouts, and radish. Glutathione is a potent antioxidant that is abundant in broccoli, and research suggests that it may be helpful in treating autoimmune illnesses. Glutathione, which also protects against oxidative stress, can ease chronic inflammation. Sulforaphane is a type of super powerful antioxidant found in broccoli in abundance. This antioxidant can reduce inflammation in your body by lowering your levels of cytokines and nuclear factor kappa B (NF-B), both molecules that drive inflammation in your body.
Study 1: Crohn’s disease. Study 2: Sulforaphane in preventing inflammation, oxidative stress and fatigue. Study3 : ageing and neuro-degeneration. We grow broccoli all year round in our vegetable garden. Can you see why?
 Cherries
CherriesCherries are not only delicious, they are a rich source of anti-inflammatory antioxidants like anthocyanins and catechins, polyphenols and vitamin C.
A study involving 37 people who ingested 16 ounces (480 mL) of tart cherry juice daily for 12 weeks had considerably reduced levels of the inflammatory marker CRP.
They have studied tart cherries more than other types for their health-promoting characteristics, but regular sweet cherries also have advantages. Research has revealed that consumption of any cherries reduced markers for oxidative stress, inflammation, exercise-induced muscular soreness and loss of strength, and blood pressure in the short term, according to published findings. A few published studies also suggest that cherries can help with arthritis, diabetes, blood lipids, sleep, cognitive functioning, and even mood.
They have shown tart cherry juice through studies to be beneficial for insomnia, and also to ease gout symptoms.
 Dark Chocolate and Cocoa
Dark Chocolate and CocoaDark chocolate is rich and can even be addictive! It’s also high in antioxidants, which aid in inflammation reduction and may lower your risk of disease as you get older. To gain the anti-inflammatory benefits, choose dark chocolate that has at least 70% cocoa or more. Chocolate’s anti-inflammatory properties are because of flavanols, which help maintain the endothelial cells that line arteries healthy. Studies have revealed that actions of chocolate include inflammation reduction, free radical reduction, enhancing the brain’s ability to form new neural connections, blood pressure reduction, and enhanced blood circulation. What many people may not know is that chocolate can also help your guy by increasing microbiome diversity. Enjoy only a small amount of chocolate daily if you have an autoimmune disease, preferably very dark chocolate.
 Extra Virgin Olive Oil (EVOO)
Extra Virgin Olive Oil (EVOO)One of the healthiest fats you can consume is extra virgin olive oil. It’s high in monounsaturated fats and a key component of the Mediterranean diet, which has a long list of health benefits. They have linked extra virgin olive oil to a lower risk of a variety of major health problems in studies, including heart disease,
CRP and many other inflammatory markers fell dramatically in those who ingested 1.7 ounces (50 mL) of olive oil per day for 12 months in one trial on the Mediterranean diet. Research has revealed that oleocanthal, an antioxidant present in olive oil, is as good as the anti-inflammatory medicine ibuprofen, making EVOO the best oil to consume if you have inflammation or wish to prevent it. Extra virgin olive oil has more anti-inflammatory properties than refined olive oil, always but Extra Virgin Olive Oil, the other olive oils don’t hold the same values.
 Fatty Fish
Fatty FishThe long-chain omega-3 fatty acids eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) are abundant in fatty fish, besides top levels of protein. Although many species of fish contain omega-3 fatty acids, these are the finest sources: salmon, sardines, herring, trevally, mackerel, and anchovies. They have conducted several clinical trials evaluating the advantages of omega-3 fish oils in humans, including rheumatoid arthritis, Crohn’s disease, ulcerative colitis, psoriasis, lupus erythematosus, multiple sclerosis, and migraine headaches. Many placebo-controlled studies of fish oil in chronic inflammatory disorders show considerable benefits, such as reduced disease activity and reduced anti-inflammatory drug use.
Your body metabolises omega-3 fatty acids into anti-inflammatory chemicals called resolvins and protectins. These compounds help prevent inflammation, which can lead to metabolic syndrome, heart disease, diabetes, and renal disease. People who ate salmon (or omega-3 supplements) had lower levels of the inflammatory marker C-reactive protein (CRP) in studies.
 Ginger
GingerGinger’s health-promoting properties are well known. It can treat a wide range of diseases via immune and anti-inflammatory responses. Because of the anti-inflammatory effect of ginger, it can reduce muscle pain after intense physical activity according to a 2103 study.
 Green Tea
Green TeaGreen tea is one of the healthiest beverages available, and fighting inflammation can be almost as easy as drinking two cups of tea each day. This wonderful tea contains catechins, which are anti-inflammatory antioxidants. Green tea also contains one of the most powerful catechins, EGCG (epigallocatechin-3-gallate), according to research. EGCG reduces pro-inflammatory cytokine synthesis and fatty acid damage in your cells, which helps to reduce inflammation. Matcha green tea is one of the best of all green teas to drink in fighting inflammation. They have linked the regular consumption of green tea to a lower risk of diseases, including heart disease, cancer, Alzheimer’s disease, obesity, and more in studies.
 Grapes
GrapesResveratrol is a polyphenol found in red grapes and red wine, among other foods and beverages. Studies have shown that resveratrol has anti-inflammatory, antioxidant, and anti-ageing properties, and when used in animal and human studies to slow the progression of autoimmune diseases like rheumatoid arthritis, systemic lupus erythematosus, psoriasis, inflammatory bowel disease, and type 1 diabetes mellitus. Adults who consumed grape extract daily had higher levels of adiponectin, according to a 2012 study. Your risk of chronic diseases like heart disease, chronic inflammatory disorders and even cancer is increased if your adiponectin is low, according to research.
 Peppers
PeppersBell and chilli peppers are high in vitamin C and antioxidants, which have anti-inflammatory properties. Bell peppers also contain the key antioxidant quercetin, that helps to lower inflammation in many chronic conditions, including diabetes, according to research.
Chilli peppers include the anti-inflammatory compounds sinapic acid and ferulic acid, which may help you age better. Bell peppers are high in antioxidants and low in starch, especially the bright red ones. Sweet bell peppers, like spicy peppers, contain the chemical component capsaicin, which helps reduce inflammation and discomfort.
 Shiitake Mushroom
Shiitake MushroomThere are many kinds of mushrooms, but shiitake mushrooms are the mushrooms besides the lion’s mane mushroom that you’d want to consider consuming when you have a chronic condition like an autoimmune disease. Research has shown that shiitake mushrooms contain abundant amounts of polysaccharides including lentinans and other beta-glucans, substances that protect your body’s cells from damage, promote white blood cell production, boost immune function and help your immune system combat pathogens. When people in a trial consumed two dried shiitake mushrooms per day, their immune system indicators improved and their inflammation levels decreased after only one month. A study conducted in 2011 showed that by eating one shiitake mushroom per day, you could improve immune function.
 Turmeric
TurmericTurmeric is an earthy, warm spice that is frequently used in curries and other Indian recipes. This beautifully coloured and fragrant spice contains curcumin, a potent anti-inflammatory agent that has received a lot of attention.
They have proven Curcumin through research to lower inflammation in arthritis, diabetes, and other conditions in studies. In one study, when people with metabolic syndrome consumed curcumin daily, along with piperine (from black pepper), their CRP, an inflammatory marker, dropped significantly in their blood.
Research suggests that curcumin can help in the management of oxidative and inflammatory conditions, metabolic syndrome, arthritis, anxiety, and hyperlipidemia. It may be difficult to get enough curcumin from turmeric to have a visible effect. Taking isolated curcumin pills may be significantly more effective. We can take Curcumin tablets at the same time as piperine, which can increase curcumin absorption by a whopping 2,000 percent.
Nutritional supplements for auto-immunity