Natural remedies for shingles offer holistic approaches to alleviate symptoms and promote healing. From soothing cool compresses and baths with baking soda to topical applications of chickweed ointment, these remedies aim to ease the pain and itchiness associated with shingles.
Natural remedies for shingles offer effective alternatives to conventional treatments, providing holistic approaches to alleviate symptoms and promote healing. From soothing compresses to dietary adjustments and vitamin supplements, these methods aim to bolster immune function and manage discomfort naturally.
Shingles, also known as herpes zoster, is caused by the varicella-zoster virus, the same virus responsible for chickenpox. After a chickenpox infection, the virus can lie dormant in nerve tissues and reemerge years later as shingles, marked by a painful rash that can significantly affect your quality of life.
This page will delve into shingles, covering its definition, causes, signs, and symptoms, while exploring both conventional and natural treatment options that offer relief. There are numerous natural treatment avenues to consider, particularly dietary changes and natural immune-boosting supplements.
Shingles occurs when the varicella-zoster virus reactivates in your body.
This reactivation can be triggered by various factors, including:
Stress: Emotional or physical stress can weaken your immune system.
Lowered Immunity: Conditions like HIV/AIDS or cancer, or treatments such as chemotherapy.
Age: Older adults are more susceptible to shingles.
Shingles is a herpes viral infection, similar to Herpes Simplex Type 1 (cold sores) and Herpes Simplex Type 2 (genital herpes). Shingles can be highly distressing, typically beginning with a tingling, sharp, burning pain under the skin. This is usually followed 2-3 days later by a red rash and blisters. Among skin conditions, shingles is one of the most painful, as it involves the underlying nerves. We’ve seen older patients suffer greatly from shingles, and I hope this page can help you identify this form of herpes and find relief.
The virus responsible for shingles, herpes zoster, is a member of the same family as the chickenpox virus (varicella-zoster). It’s widely accepted among experts that shingles can manifest years after an initial chickenpox infection because the virus can lay dormant in nerve cells near the spinal cord. From my clinical experience, I’ve noticed that shingles tends to be more aggressive in individuals who either suppressed an early chickenpox infection with medications or had an incomplete manifestation of chickenpox symptoms. All herpes viruses, including those causing cold sores or genital herpes, persist in the body for life. These viruses have the potential to reactivate when a person’s immune system weakens due to various factors, which we will explore further.
Shingles can occur at any age but usually affects all genders equally. Those at greater risk include individuals with impaired immune systems due to ill health, medications, or diseases affecting the immune system.
– Burning, Stinging Pain: Shingles commonly affects one side of the body. The pain, described as tingling, sharp, or burning, can occur anywhere but often affects the face, upper abdomen, or back. Pain severity can increase with age and the duration of shingles.
– Symptoms Accompanying Pain: Other symptoms include fever, a sensation of being hot, cold, or clammy, headache, upset stomach, and tender or enlarged lymph nodes around the neck, groin, or armpit.
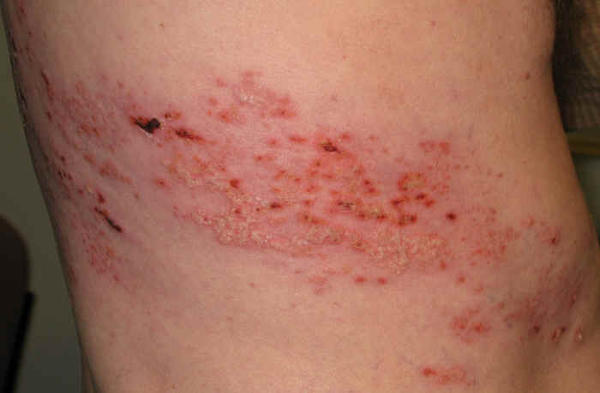
– Skin Rash: Initially, you may develop a fever and tender or swollen lymph nodes near the rash site. A red rash appears 2-3 days later over the painful area, followed by small, fluid-filled blisters. The rash can be extremely itchy. Blisters typically dry and crust over within a few days, clearing up completely within 2-3 weeks, though severe cases may cause mild scarring.

Some patients find relief from itchiness with hot water or cold packs; however, during the acute blister stage, hot water may be unbearable.
Infectivity and Transmission
Herpes is most infectious when blisters are present. Avoid scratching blisters to prevent spreading the virus to others. Shingles affects nerves, and the rash often appears in a band across the body or down the leg along the affected nerve. In some cases, a rash may not develop after the initial pain.
I hope this information helps you understand shingles and find ways to manage it effectively.
Diagnosing shingles is typically straightforward for an experienced practitioner who can recognize the condition based on its distinctive symptoms. Throughout my years of practice, I’ve encountered numerous cases characterized by fever, pain, and a specific rash that were later confirmed to be shingles.
Most doctors can diagnose shingles by observing these symptoms alone. A comprehensive medical history will be taken, and your healthcare provider might also collect fluid from the blisters for laboratory testing to confirm the presence of the shingles virus.
There are many potential causes of shingles, but is is thought that these factors have the most influence on the development of shingles:
Read our article on Stress and the Immune System here
Conventional medical treatment for shingles primarily aims at alleviating symptoms, as antibiotics have minimal effect on the virus and antiviral drugs offer limited relief. In rare cases where shingles affects the eyes, prompt treatment by an ophthalmologist is essential to prevent damage to the cornea, the eye’s transparent covering over the iris and pupil.
Your doctor may recommend several typical treatments, including:
– Applying cool compresses to the affected area.
– Using pain relief medications like Ibuprofen or Paracetamol.
– Applying lotions or creams to soothe the rash.
– Prescribing antiviral drugs like Acyclovir, which offer limited impact on the virus.
– Administering steroids such as Hydrocortisone for severe rash and pain.
– Utilizing antibiotics if the skin rash becomes infected, leading to bacterial complications in the affected area.
I always recommend washing the shingles lesions a few times a day with Tea Tree Oil Soap and then leaving them uncovered to breathe. It’s important to note that the shingles virus can be passed to another person who has not had chickenpox via the open rash during the blister phase, so it is crucial to cover the sores.
A cool, wet compress applied to the blisters can help relieve pain and itching associated with shingles. Compresses can be made in two ways:
1. Water Compress: Simply use water by itself.
2. Vinegar Compress: Create a compress using water and apple cider vinegar by adding about a tablespoon of vinegar to a liter of water.
Compresses should be applied three times a day while the pain and itching persist.
Cool baths are another soothing anti-itch solution that provides relief. Additionally, adding baking soda to the bath helps with itching. Similarly, uncooked oatmeal can be used in cool baths to alleviate itching associated with shingles. This relief from these symptoms is important as it prevents scratching blisters, thereby potentially causing scarring or infection.
Chickweed Ointment, found in health-food shops, can be highly beneficial in soothing itchiness, especially after the fluid-filled vesicles have burst and crusted over.
There are many different natural health options available for herpes viruses, both for prevention and treatment. Here are some of the best solutions:
A simple trick to relieve lesions is to apply a cool or cold wet washcloth to the affected area. A wet towel can be put in the freezer for a while to make it colder. Apply ice if you feel a herpetic lesion coming on.
Heat can also be a great relief to some people. A warm to hot shower or bath has provided relief for some of my patients. It’s worth trying if the cold does not provide relief.
Vitamin C is one of the best vitamins, and I suggest taking it when diagnosed. A good daily dose is much more effective than Acyclovir. Start with half a teaspoon of Vitamin C powder twice daily and build up to three doses of half a teaspoon daily.
Taken daily before meals, Vitamin E may reduce the pain of shingles. These capsules of Vitamin E can be squeezed directly onto lesions to help with pain.
A study published in the Journal of Geriatrics showed that Vitamin B12 injections were beneficial.
Calamine lotion may relieve the pain and help dry the lesions.
Acupuncture has been shown to be most beneficial for nerve pain. Give it a go if the pain is chronic.
Tai Chi: According to the National Centre for Complementary and Alternative Medicine, Tai Chi has been found to boost the immune system in older adults, aiding shingles. Tai Chi is a traditional form of Chinese exercise combining relaxation, meditation, and aerobic activity, often referred to as “meditation in motion.” A clinical trial at the University of California, Los Angeles, suggested that Tai Chi might not only help older adults boost their immunity to shingles but also reduce the severity and duration of this immune problem.
Take a Chill Pill: According to the Mayo Clinic, regular periods of rest and avoiding strenuous activities are highly recommended for those feeling weak or tired from the pain of shingles. The Mayo Clinic also recommends avoiding stress, which can worsen pain. Techniques like listening to music or other relaxation methods can be helpful.
Distraction: Distraction is another technique to diminish the discomfort of shingles pain. Focusing on pain and itching can lead to stress or obsessive scratching, potentially causing infection. Engaging in hobbies or reading can help take the mind off the condition.
Reducing stress levels and getting adequate rest are most important. A diet full of fresh fruits and vegetables is the best starting point for both prevention and treatment of shingles.
Eliminate sugars from your diet as sugar directly suppresses your immune system.
A diet rich in vitamins, minerals, and various nutritional factors has a tremendous ability to boost your immune system. Brightly colored fruits and vegetables are best – think capsicums (bell peppers), eggplant, carrots, avocado and red onions.
Some misguided advice claims that “protein can encourage herpetic blisters and symptoms, and if you eat protein, take the amino acid supplement Lysine to counteract the amino acid Arginine found in protein linked to cold sore activation.”
This is complete nonsense. The appearance or aggravation of a herpes condition is not linked to animal meats like chicken, fish, or beef. In fact, chicken and fish are rich sources of Lysine, which inhibits herpes viral replication. In my experience, the worst foods for those with herpes is chocolate and nuts. And this includes the hazelnut and chocolate spread Nutella.
My dietary recommendations are specially formulated for those suffering from herpes-type viruses, including Herpes 1 (cold sores), Herpes 2 (genital herpes), Shingles, and Chicken Pox.
Avoid or eliminate foods containing Arginine, which aids in viral replication, especially during an outbreak. Eat foods high in Lysine, which inhibits viral replication. This approach is particularly effective when used in conjunction with the diet and additional Vitamin C.
– Chocolate & Carob
– Cocoa & Milo
– Nuts (peanuts, almonds, pecans, walnuts, macadamia)
– Rice
– Corn
– Barley
– Rye
– Buckwheat Flour
– Whole oats
– Sesame seeds
– Sunflower Seeds
– Gelatin Jelly
– Coconut
– Chicken
– Beef
– Fish
– Soy protein (soybeans, tofu)
– Acidophilus yogurt
– Hard cheeses (moderate)
– Eggs
– Figs
– Dates
– Tomatoes
– Peaches
– Turnip
– Asparagus
Shingles is not always contagious; it is only infectious during a specific stage. The varicella-zoster virus, which causes both shingles and chickenpox, can spread from person to person, primarily through direct or indirect contact with the fluid in shingles blisters. During the active phase of shingles, when blisters are present, the virus can be transmitted to others, potentially causing chickenpox.
The virus remains dormant in nerve tissue indefinitely after the initial infection, but it can reactivate years later, leading to a recurrence of shingles.
Shingles can lead to several complications, though most are rare.
1. Post-Herpetic Neuralgia: This is persistent pain at the site of the shingles rash lasting more than one month. Anti-seizure and anti-depressant medications may be used to treat this pain.
2. Bacterial Skin Infections: The affected area can become infected, requiring antibiotics.
3. Eye Damage: If shingles affects the eye and is left untreated, it can cause damage to the cornea. This can potentially lead to blindness.
4. Foetal Damage: Shingles in early pregnancy can damage the fetus. However this is very rare.
Post-Herpetic Neuralgia
Post-herpetic neuralgia refers to nerve pain experienced after shingles. Results can be variable and may be disappointing in long-standing cases.
Here are the best tips:
– Vitamin E: 400 IU, 3 times per day for prevention or treatment. Long-term administration may be necessary for established neuralgia.
– Vitamin B12 and Thiamine: 1,000 mcg and 50 mg intramuscularly, daily, then taper according to response (anecdotal).
– Topical Capsaicin (0.025%): Apply 4 times per day for treatment. In an uncontrolled trial, this treatment reduced or eliminated pain in 9 of 12 patients after 4 weeks. Capsaicin may cause transient burning after each application for the first 3 days. Avoid contact with the eyes; application with a gloved hand may be desirable.
– For Herpes Zoster Ophthalmicus: Eyedrops containing Vitamin C (250 mg/ml) and Vitamin A (2,500 IU/ml), adjusted to physiologic pH. Place 1-2 drops in the eye every hour; taper as improvement occurs (clinical observation – Dr. Jonathon Wright).
– Doermann, D. J., & Frey, R. J. (2006). Shingles. The Gale Encyclopedia of Medicine, Third Edition. Jacqueline L. Longe, Editor. Farmington Hills, MI: Thomson Gale.
– DermNet NZ (2007). Shingles. New Zealand Dermatological Society.
Shingles on face, how long does it last after first blisters?
Depends on your diet and lifestyle! You can nail these blisters in under ten days
Some articles say Don’t eat tomatoes, then others say it’s ok, which one is correct? Some say canned tuna is good, others say it’s not, Does anyone really know any blog answers??
Kia ora Frank,
Thanks for your comment and for visiting our site! We’re big fans of the Mediterranean diet and don’t subscribe to the lectin theory. You’ll find plenty of delicious tomato recipes on our site! 😊
Regarding canned tuna, we do have some concerns, particularly about mercury levels, but moderation is key. It can still be part of a balanced diet. Ngā mihi, Tracee