Osteoarthritis (OA) is the most common form of arthritis. It is a degenerative disease affecting the whole joint, and any joint can be affected but OA most commonly affects the knees, hips, hands, neck and low back. Diet changes, vitamins, minerals, and herbal medicines can all help significantly.

The term “osteo” means bone, and “arthritis” means inflammation of a joint. There are as ways that people can experience arthritis as there are types of arthritis. There are literally dozens of kinds of arthritis: osteoarthritis, rheumatoid arthritis, gout, systemic lupus, bursitis–to name just a few. The good news is that arthritis will rarely kill you, although the pain can well and truly drive you up around the bend. The bad news is that the stiffness that you experience can make you feel like real old age has set in far too early.
Osteoarthritis (OA) is the most common form of arthritis. It is a degenerative disease affecting the whole joint, and any joint can be affected but OA most commonly affects the knees, hips, hands, neck and low back. Diet changes, vitamins, minerals, and herbal medicines can all help significantly. OA can be isolated to one joint, generally a weight bearing joint such as the hip or knee, but it often affects multiple joints. OA can lead to significant problems with mobility with middle aged and elderly people and is probably the most common cause of disability in elderly people in the developed world. OA affects so many people, and I have often been asked to write about it by patients, and offer some of the best natural medicine solutions I know. Let’s explore this condition and see what we can offer, there are many options and I’ll try to give you plenty.
Sir William Osler, known as the “Father of Modern Medicine,” once said, “When an arthritis patient walks in the front door, I feel like leaving by the back door.” After seeing many arthritic patients over the years, I can sympathise with Dr. Osler and understand that many other conventional medical doctors since him have difficulties facing arthritic patients, because there is little that conventional medicine offers them apart from drugs and surgery. I trust that the following points do not come across as being too cynical, it is just my experience in dealing with patients with arthritis who rely primarily on conventional medicine for arthritis treatments:
 Anybody who is alive and active will probably develop a wear and tear syndrome affecting the mechanical parts of their body like their joints sooner or later.
Anybody who is alive and active will probably develop a wear and tear syndrome affecting the mechanical parts of their body like their joints sooner or later.
Do you own a motor vehicle? Then it is realistic to understand that if you owned your vehicle for 50 or 60 years or so (the time when osteoarthritis generally will present itself) that if will show signs of significant wear and tear in those shock absorbers (your knees), the chassis (your spine) or perhaps your hips (or shoulders (axels, wheel bearings, etc).
The fact is, the older we get, the more likely it will be that something just plain wears out. But this is certainly not true for all motor vehicles! Perhaps your vehicle was the type that was just driven to church on a Sunday? Or maybe your car was washed and polished every week, had an oil change and service twice yearly and was carefully driven and parked? Then maybe you belong to that group that never has a problem all through their life with the human frame. There are many reasons why people don’t develop osteoarthritis, and my guess would be that there are just as many reasons why they do.
For many years I have seen certain patients hobble around with sore knees and hips. They could be the kind of people who were very active in their younger years or they could be people who just plain wore out their joints from excessive exercise, or had an accident, a fall, etc. Either way, there is often a history of unusual activity surrounding the affected joint/s in those with osteoarthritis. You may also find that those with OA are the perfectionist people, or like to take control and do things their way. They may do too much and feel happier for having done things “their way”, and this kind of behaviour will ensure that they simply do too much and wear their bodies out prematurely.
 Typically, if a guy tells me that he was a truck driver for years (getting in and out of the cab) or a bricklayer (very hard on the joints) or even a mechanic (bending down on knees and looking/working under vehicles) these are all cases for osteoarthritis later in life. A football player, a person who works as a gardener, or even a dressmaker can develop arthritis. You will typically find the “weekend warriors” or the sporting enthusiasts will often develop arthritis.
Typically, if a guy tells me that he was a truck driver for years (getting in and out of the cab) or a bricklayer (very hard on the joints) or even a mechanic (bending down on knees and looking/working under vehicles) these are all cases for osteoarthritis later in life. A football player, a person who works as a gardener, or even a dressmaker can develop arthritis. You will typically find the “weekend warriors” or the sporting enthusiasts will often develop arthritis.
Just like stress and anxiety are often a cause of muscular pain and tension, excessive use of a limb can result in wear and tear causing osteoarthritis. You get the picture – those who simply do too much or expect too much from their bodies are more likely to end up with arthritis than those who take it easy and slow down when they feel their body needs a rest. That is not to say that all cases of arthritis are caused this way, there are many potential causes of osteoarthritis. Osteoarthritis is also known as a “degenerative” arthritis or the “wear and tear” arthritis. If you’ve been told by your doctor that you have this type of arthritis, there’s a good chance you can substantially reduce or even eliminate your symptoms, while tapering down or even eliminating drugs you may be taking.
A number of predisposing factors can hasten this degenerative process, even in young people.They include:
The most commonly affected joint is the knee joint, and the second most commonly affected is the hip joint. As mentioned earlier, it is the hips, knees, ankles, neck, low back and hands in general which are the most commonly affected joints. Hip pain can be especially severe, even making walking extremely painful and difficult. Some people’s fingers may develop a knobby and gnarled appearance (Heberden’s nodes). Osteoarthritis of the spine is a common cause of chronic pain and decreased neck and back mobility. In some cases, large bone spurs may compress the spinal cord or pinch its nerve.
Did you know there are several stages of knee arthritis? In stage 1 you’ll have wear and tear in the knee joints and probably won’t experience much in the way of aches of pains on the knee. In the severe stage, stage 4, You knee cartilage is almost gone, making your knee very stiff and painful, even requiring surgery. Those with knee arthritis in the moderate stages of cartilage degeneration may notice more pain with walking and especially running, kneeling and squatting.
Osteoarthritis is usually experienced as aching joints and stiffness. The pain is aggravated by movement and weight-bearing on the involved joint. The osteoarthritis sufferer may feel worse when they are cold or with little movement. As they warm up, the joint may not feel quite as bad and even improve a little with mild exertion. This is not always the case however, as it may aggravate significantly and may even feel much worse for continued motion.
With rheumatoid arthritis however (the inflammatory type of arthritis) this will not be the case. Although swelling may occur with OA, warmth and redness and heat of the affected joint usually imply an inflammatory-type of arthritis like rheumatoid arthritis (RA) or gout.
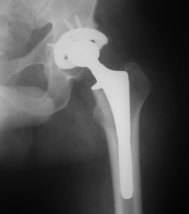 Did you know that almost 85% of all knee and hip replacements are carried out because of osteoarthritis? You replace your car, your toothbrush, and other items commonly used on a regular basis. Some folk even change their partners on a regular basis, but you don’t replace your joints, they just keep on going day after day, year in and year out. Some of us may get a knee or a hip replacement, and for some, it is the only way to improve the quality of their lives when the pain is just too much to bear.
Did you know that almost 85% of all knee and hip replacements are carried out because of osteoarthritis? You replace your car, your toothbrush, and other items commonly used on a regular basis. Some folk even change their partners on a regular basis, but you don’t replace your joints, they just keep on going day after day, year in and year out. Some of us may get a knee or a hip replacement, and for some, it is the only way to improve the quality of their lives when the pain is just too much to bear.
In my experience, I have found that some patients ended up replacing the opposing joint down the track. The problem is that the corresponding joint to the one replaced (the healthier one on the other side of the body) may take more strain and may need attention in due course. Your mechanic would rather replace both brake shoes and shock absorbers on your car when only one needs replacement, or both tyres are replaced simultaneously as a set rather than one at a time. Why? Because your mechanic can see the need for balance, a brand new tyre on one side of your vehicle may act and respond differently (more favourably) in various driving conditions. Replacing both tyres at the same time ensures that you don’t place unnecessary strain on your shock absorbers and other parts of the car’s driving train. Similarly, if only one hip is replaced, or one knee joint, you may end up with lower back or knee problems, I’ve see this happen on many occasions. If you do have a knee or hip replaced, take it easy for at least 3 to 6 months and I’d highly recommend a course of Feldenkrais or Tai Chi to bring about more balance and harmony to your body’s scaffolding. Common sense? I think so, and it is often lacking in medicine. I’m certainly NOT advocating that you get both hips or knee joints replaced at the same time, this is simply not feasible or even possible in most situations.
Osteoarthritis is like any chronic ongoing health complaint you may have, it will be aided by superior nutrition. Nutritional factors are very important in the successful treatment of arthritis, and it is important to focus on foods to avoid as they may well aggravate arthritic problems. Let’s take a look at food allergies and the nightshade family of foods.
 The nightshade family includes tomatoes, potatoes, peppers (capsicum), chilli, and eggplant along with tobacco in any form. I have found over the years that a sensitivity to certain natural chemicals called alkaloids (naturally present in the nightshades) only cause pain and swelling in a minority of individuals with arthritis. The problem with nightshade sensitivity is that it is not detectable by any current laboratory tests, so you will only determine this by trial and error, and the only way to figure out whether nightshade vegetables bother you is to totally eliminate them.
The nightshade family includes tomatoes, potatoes, peppers (capsicum), chilli, and eggplant along with tobacco in any form. I have found over the years that a sensitivity to certain natural chemicals called alkaloids (naturally present in the nightshades) only cause pain and swelling in a minority of individuals with arthritis. The problem with nightshade sensitivity is that it is not detectable by any current laboratory tests, so you will only determine this by trial and error, and the only way to figure out whether nightshade vegetables bother you is to totally eliminate them.
Even if you believe that you are nightshade sensitive and totally eliminate all of these, it can still take three to four months for symptoms to recede. I have found in my clinic over many years that only a handful of those who have entirely avoided nightshades have ever noticed significant relief.
Many natural medicine practitioners automatically exclude nightshade family foods from a person’s diet if they complain of OA or RA (rheumatoid arthritis) as if it is “standard treatment” in naturopathic practice. In my practice, firstly I like to see how much of the nightshade the person consumes, in what form/s and if it is possibly connected to their aggravations. The problem with many “self-help” books the internet with regard to health related information is that one website may simply regurgitate information from another website, and so the nonsense is perpetuated.
Mark Twain once said: “Be careful when reading health-books, you may die of a misprint”. If Mark Twain lived today, he would have meant “Be careful when browsing the internet and viewing websites”. I question how many people who set these sites up ever see patients with arthritis to know whether nightshades really cause the pain and aggravations they claim. Would I exclude nightshades from a person’s diet who complains of arthritis?
Possibly, but then I probably would exclude just the one night shade food from that person’s diet they consumed the most, and then only after having worked with the Hypoallergenic Diet and having repaired the digestive system first. This to me is like taking a person off all gluten and wheat products before you eliminate dairy products, peanuts and the most likely allergenic foods first. And remember, nightshade sensitivity is that – a sensitivity, NOT an allergy.
Food allergies have nothing to do with nightshade sensitivity. Immediate (IgE) and delayed (IgG) food allergies can cause all sorts of grief for the patient, and in my opinion are more of an issue than nightshade sensitivities. I have certainly seen many OA patients improve their pain levels after being placed on a “low-allergy” diet.
I have a special Hypo-Allergenic Diet sheet which I give to patients who see me, it has proven to be very effective and pinpoints the foods you are most likely to react to. If you’ve had allergies in the past, have them now, or if a member of your family has allergies, this is a definite possibility. But why would allergies increase the inflammatory responses, how is it linked? This is easy to explain, especially if you have a history of “pain killers” like Paracetamol, Ibuprofen, or various other drugs your doctor may have recommended. Such drugs dramatically affect your digestive system over time, and one of the biggest issues your small bowel will face is “leaky bowel syndrome” where the small intestine becomes “leaky” or permeable allowing tiny protein molecules to come into contact with your immune system more readily, setting up an antigen-antibody response. What this means in English is that your immune system will come into contact with foreign molecules from your diet which it isn’t supposed to. When this occurs, chemicals are produced in turn by the immune system which in turn wreak havoc on your system and produce symptoms like pain and inflammation.
A good tip for you is to go on a ten-day cleanse which can bring about symptom relief, and sometimes dramatic. If you do find relief in the ten day period then it’s very likely you have significant food allergies. If this occurs, then I’d highly recommend you stay on the Hypo-Allergenic Diet for 3 months.
 Exclusion diets produce the best results in the earlier, more painful stages of the drawn out disease process known as flavourings and any long-term chronic health complaint, it will be found that there is a balance that must be found between a rigid nutritional program that might not be effective, as well as eating habits that have a positive psychological effect on the person. I try to achieve this in a clinical sense, but it can be a real challenge at times with some people.
Exclusion diets produce the best results in the earlier, more painful stages of the drawn out disease process known as flavourings and any long-term chronic health complaint, it will be found that there is a balance that must be found between a rigid nutritional program that might not be effective, as well as eating habits that have a positive psychological effect on the person. I try to achieve this in a clinical sense, but it can be a real challenge at times with some people.
Try these following exclusion suggestions for 3 months to see if they have any effect on your arthritis:
 Mainstream medical treatment for degenerative arthritis includes aspirin, other non-steroidal anti-inflammatory drugs, synthetic forms of cortisone both swallowed and injected, and surgery. Although all of these drugs relieve symptoms, there is increasing evidence that they accelerate the deterioration of cartilage and actually make the underlying condition worse. I spent six years after qualifying as a naturopath working in conjunction with a British doctor who said that steroid injections in and around a joint was a ridiculous thing to do and a “medical travesty”. I couldn’t agree more, it gives temporarily relief only and ends up destabilising the joint in time. The patient gets a false sense of security, they think that the arthritis is cured. Their arthritis is no more “cured” than a mortgage is paid for by credit, it is only deferred to a later time when it becomes increasingly inconvenient to pay back the debt.
Mainstream medical treatment for degenerative arthritis includes aspirin, other non-steroidal anti-inflammatory drugs, synthetic forms of cortisone both swallowed and injected, and surgery. Although all of these drugs relieve symptoms, there is increasing evidence that they accelerate the deterioration of cartilage and actually make the underlying condition worse. I spent six years after qualifying as a naturopath working in conjunction with a British doctor who said that steroid injections in and around a joint was a ridiculous thing to do and a “medical travesty”. I couldn’t agree more, it gives temporarily relief only and ends up destabilising the joint in time. The patient gets a false sense of security, they think that the arthritis is cured. Their arthritis is no more “cured” than a mortgage is paid for by credit, it is only deferred to a later time when it becomes increasingly inconvenient to pay back the debt.
The treatment of osteoarthritis depends on how far advanced the condition is. In the early stages, treatment for osteoarthritis is usually directed at decreasing the inflammation in the joint. Anti-inflammatory medications, such as aspirin and ibuprofen, are used in decreasing the pain and swelling from the inflammation. It pays to start with a more natural treatment approach you experience severe pain, rather than having high expectations of natural medicines acting like a strong painkilling drugs, which they don’t. Every OA patient will gain some benefit from a good quality vitamin C formulation. There are different natural options however, and these should be tried initially before resorting to drugs which have side-effects. The other product we recommend in our practice and which is a favourite by many is Boswellia Resin Extract.
If the symptoms continue, a cortisone injection may be used to bring the inflammation under better control and ease your pain. Cortisone is a very powerful anti-inflammatory medication, and does have secondary effects that limit its usefulness in the treatment of osteoarthritis. The major drawback in the use of intra-articular injections of cortisone is the fact that it may actually speed the process of degeneration when used repeatedly. I highly recommend that if you do contemplate cortisone, that you use it most sparingly, and definitely avoid multiple injections.
NSAIDs (Non-Steroidal Anti Inflammatory Drugs): these can be used if paracetamol and/or topical NSAIDs to provide insufficient pain relief. Standard NSAIDs or “COX-2 inhibitor” drugs are often first choice. They should be co-prescribed with a proton pump inhibitor. Proton pump inhibitor drugs (PPIs) are a group of pharmaceutical drugs that decrease the amount of acid in the stomach and intestines.
Doctors prescribe PPIs to treat people with recurring reflux, ulcers in the stomach or intestine, or other digestive disorders that may cause excess stomach acid like taking a regular drug to “kill” the pain of arthritis. Now instead of taking one drug, you are taking two, and it doesn’t take a rocket scientist to figure out that it may not be the smartest thing to “block” stomach and intestine acid production because you need that stuff to digest and absorb food. And – if you digestion doesn’t work favourably, how on earth can you ever rebuild and repair a dysfunctional joint? You will always stay symptomatic and look for those “pain-killing” pills.
A referral for joint surgery should be considered for people with joint symptoms (pain, stiffness and reduced function) that:
 My article has reviewed a number of promising alternatives for the prevention and treatment of OA. Although additional research into the most effective natural treatments for OA needs to be done, some of the treatments discussed appear to be as effective as, and even better tolerated than conventional drug therapy. In addition, preliminary evidence (such as the persistence of improvement after treatment is discontinued, and positive findings or X-ray and biopsy findings) suggests some of these treatments may even help to arrest or reverse the arthritis disease process.
My article has reviewed a number of promising alternatives for the prevention and treatment of OA. Although additional research into the most effective natural treatments for OA needs to be done, some of the treatments discussed appear to be as effective as, and even better tolerated than conventional drug therapy. In addition, preliminary evidence (such as the persistence of improvement after treatment is discontinued, and positive findings or X-ray and biopsy findings) suggests some of these treatments may even help to arrest or reverse the arthritis disease process.
Is the stiffness in your character, literally creating stiffness in your body? In my clinical experience, some arthritis patients are unbend able and stiff in their approach to life, unyielding and unable to change or accept change in their lives. Are you resisting inevitable change in your life?
Loosen up. Say to yourself: “I expect change, and I will bend with this change. Be like bamboo – stay strong, yet have the ability to bend and flex easily if the wind comes up from nowhere. That way you won’t break when challenged!
Walk, don’t run. As you get older, it becomes easier to become more complacent about activity. It is easier to watch television than to go outside for a walk, have you noticed? A range of motion exercises are very important to increase circulation and reduce stiffness. With rheumatoid arthritis, you should avoid exercising a joint that is inflamed or “hot,” but even in these cases these joints can be gently moved along their range of motion. Swimming is a particularly good exercise for people with all forms of arthritis. Personally, I am NOT a big fan of running or jogging, even though it is not associated with degenerative joint disease, you might like to consider walking as an alternative form of exercise if you experience any joint pain during or after jogging. I find it quite hard on the body, and prefer brisk walking, especially uphill. I walk daily with my wife at a beautiful nature reserve close to where I live, we take our dog and I really enjoy the experience. It is important not to overdo any exercise, but don’t under do it either.
Weight loss. Are you carrying too much weight? Then how can you expect no knee or back pain if you are overweight? One of the first things a person tells me who has lost a lot of weight is that their back and knees don’t hurt that much anymore. Funny that. I should have a bag of two of potatoes in my room, and hand them to the person who has lost that amount of weight, they would be shocked to see how much their joints hurt at once.
Pool walking. Do you have back pain, hip or knee pain preventing you from walking? – Then try pool walking, that’s right, walking in a pool waist or chest deep. It works, and is a lot less painful than walking without all that water supporting your body. I don’t like excuses, sorry, I’ve heard them all before, like “I can’t swim” or “the water is too cold”. Try to exercise 15-20 minutes a day, five days a week. On the weekends go outside, a beach walk for a few miles going barefoot in the sand is particularly beneficial for your spine and hips. The fresh air will do you good too. Rest is rust, you simply MUST engage in life to remain fit and well as the years roll by.
Although junk and potential allergenic foods are not thought to “cause” arthritis, they may “cooperate” with it. Even though I am not convinced about the need to avoid the nightshade vegetables, there is some merit in avoiding certain groups of foods to ensure they do not play a role in aggravating your condition.
Optimise digestion. Your digestive system needs to be operating very well in order to break down and absorb the nutrients you need to repair and rebuild that cartilage around your arthritic joints which is failing you. If you are over 40, creeping up to fifty or older, then go on a course of Digestive Enzymes. You may well have an underactive stomach and small intestine, something we commonly see with OA patients.
Throw out the trash first. The first port of call with your diet is to throw out the trash, that is, the obvious junk and garbage you KNOW you shouldn’t be eating or drinking. This includes alcohol, chocolates, sweets and candies, twinkies and other such garbage foods like donuts, etc. You know they are bad, why eat them?
Avoid the allergy potential foods secondly. As I mentioned earlier, stop the allergenic foods FIRST, and before you do this stop the nightshade group of vegetables in your diet. How can you expect to get well from a disease which is causing your joints to fail, if you fail to improve your digestive system?
Avoid nightshade vegetables last. Avoid foods from the nightshade family as a last resort, including tomatoes, eggplant, bell peppers, aka capsicums (except black pepper), and potatoes (except for the potato juice, as discussed below). Do you smoke? You may need to know that tobacco is also a member of the nightshade family which can potentially aggravate arthritis.
Alkalise the body
An old folk remedy for arthritis is to drink raw potato juice. To make it, wash a potato (don’t peel it), cut in into thin slices, place it in a glass of cold water, and leave it overnight. Drink this water in the morning on an empty stomach. Another trick, especially good with inflammatory arthritis, is to juice a small whole potato each day and drink the juice. It is very alkaline and appears to have a most beneficial effect in those who have had a diet rich in breads, meats, alcohol and other acid forming foods. Cabbage juice will give a similar effect. Some evidence suggests that magnesium bicarbonate (1.5 liters of magnesium bicarbonate-containing water per day for at least six weeks) may cause the remission of osteoarthritis (by counteracting the acidosis (acidity) that may cause osteoarthritis).
Eat anti-inflammatory foods. These include turmeric, ginger and particularly pineapple. Pineapple when eaten fresh regularly will supply the body with bromelain, an enzyme which is excellent for reducing inflammation. To be effective, the pineapple must be fresh, because canning and freezing affects bromelain.
Eat more Sulphur containing foods. Sulphur containing foods include asparagus, eggs, garlic, and onions. Sulfur is required for the repair and rebuilding of bone, cartilage and connective tissues in the body, and aids in the absorption of calcium. Other good foods to eat are green leafy fresh vegetables, containing high levels of Vitamin K as well as non-acidic fresh fruits (apart from pineapple which is acceptable), whole grains, oatmeal, brown rice, quinoa, and fish.
Yoghurt can help prevent and heal arthritis. probiotics, a probiotic (friendly) bacteria found in yogurt offers “remarkable preventive and curative” effects on arthritis, say Israeli researchers in a study published in the Journal of Nutrition. Because lactobacillus has already demonstrated beneficial effects in other inflammatory diseases such as inflammatory bowel disorders, researchers thought it might also lessen the inflammation of arthritis. To find out, they ran two groups of animal experiments. In both sets of experiments, laboratory animals fed the yogurt with large amounts of lactobacilli had the least amount of arthritic inflammation, while those fed plain yogurt experienced only moderate inflammation. The animals that received just lactobacillus, even heat-killed lactobacillus, also showed significant benefit. Milk, however, had no effect. So impressed were the researchers with the study’s results that they recommended trials using commercial yogurts containing lactobacilli in arthritic patients! View Eric’s Yoghurt Recipe here.
Hydrate Your Body. Hydrotherapy is very effective in many cases for pain relief. By stimulate circulation in the affected areas through taking a hot shower or bath, then turning on the cold water, you are improving the blood flow and reducing stiffness to the arthritic areas. Repeat the warm, and then a hot cycle and then return to the tepid and cold cycle. If your hands, knees or feet are the primary sources of pain, you can place them in a tub or sink of hot and then cold water. Another alternative is to place a hot pack on a specific area and alternate with a cold pack. Try this at least twice a day. Keep a few ice packs in the freezer. Wheat bags are good too, they can be placed in the microwave for an instant heat. Do you have a microwave? Don’t use it for cooking food, but they are a great tool for reheating wheat bags!
Aerobic Fitness, Flexibility and Muscle Strength. These are the three key areas you need to improve, particularly as you age and are over 50 years like me. Those who keep good heart and lung fitness, stay flexible and are strong in their muscles have much less chance of being affected by arthritis. I had a severe motorcycle accident in 1991 and damaged my left hip and left knee cartilage significantly, yet I have very little trouble today from this previous injury due to my exercise and healthy lifestyle. Had I failed to maintain a healthy nutritional intake and avoided exercise, I have no doubt that I would have required a replacement hip and knee by now.
Keep walking DAILY, no excuses – I’ve got no time for exercise” “I’m overweight and my knees hurt” or “It’s raining outside, it’s too cold/hot, etc” “I haven’t got the time” or “I’m too old” is another lame one. Stay flexible, do you feel stiff every time you get off that couch or chair? Then it’s time to do some stretching excercise and there are plenty you can do. Men are particularly prone to stiffness and loss of flexibility as they age, a lot more so than women in my opinion.
Try Tai Chi, yoga or any one of a hundred other forms of exercise which keep you flexible and supple. This will prevent injury to a large degree. And finally, keeping your muscles strong and toned is very important also, you tend to gain more fat and lose muscle tone as you age. But how do you achieve nice muscles? Do you need to pump iron and spend countless hours in front of mirrors in the gym? No you don’t.
Try team sports or just plain swimming, cycling, or any one of a dozen similar activities which engages your muscles very regularly. I find that brisk walking up hill does the trick for me. It firms and tones the backside and legs, the largest muscles in the body.
Massage. It doesn’t take a rocket scientist to know that massage is good for people with arthritis. For the best results, avoid massaging directly on top of an inflamed joint. Instead, massage just above and below the joint. Massage improves circulation, makes you feel good and is relaxing. Have one to two sessions a week.
Identify the pressure points. Press a pressure point that is near, but not on top of, the primary source of pain. You can find a good pressure point by feeling a slight crease in the skin (it will probably be tender). Press this point for three to five seconds, let up for a bit, then press it a couple more times in a similar manner. Some other good pressure points may be close to (not directly on) nearby joints. Try to press firmly but not too hard. Breathe into it; you will find that the pain reduces, and use a portable massager to give your body a burst of energy at these points. Most effective when used daily over a sustained period of time.
Castor oil treatment. Make a castor oil pack and place it on a joint where there is pain, but not when there is acute pain and inflammation. To make this poultice, pour three or four tablespoons of castor oil in an old pan, heat the oil until it is quite warm, and then saturate a flannel cloth with the oil. After you place this cloth on the affected joint, cover it with some cling film and then a larger (old) towel and place a heating pad (hot water bottle or hot wheat pack) over it. Keep it in place for 30-60 minutes.
Copper may help. Some people I know who suffer from arthritis have been known to experience relief when they wear a copper bracelet. Although skeptics point to this treatment as a classic example of “quackery”, it is known that some people with arthritis have difficulty assimilating copper from the food they eat. Perhaps wearing a copper bracelet provides them with an additional source of this mineral, either way, I seen some remarkable turnarounds with a few patients wearing copper. Don’t knock it until you try it!
A number of natural substances may have value for the prevention and/or treatment of OA. Some of these compounds have been shown to provide symptomatic relief, and preliminary evidence suggests some may positively affect the progression of the disease. Although much of the research is in its early stages, the possibility that natural substances can be used to prevent the degradation, or enhance the repair, of joint cartilage is both encouraging and intriguing. I would like to focus on some of the more promising and popular natural medicines.
Find a product which contains Glucosamine sulfate, Chondroitin sulfate, MSM and Ginger. It has an excellent effect in those with osteoarthritis, and I recommend 1 capsule three times daily with foods.
Glucosamine sulfate (GS). GS was significantly more effective than placebo at reducing pain and improving function, and was at least as effective as NSAIDs (numerous double-blind trials). Improvement was seen typically within 4 – 6 weeks. GS may help prevent damage to articular cartilage and promote its regeneration. At least 2 long-term studies have shown that GS slows disease progression, as determined radiographically. GS (2,000 mg/day for 12 weeks) was found to improve “regular knee pain” (presumably due to previous cartilage damage, and possibly osteoarthritis) in one double-blind study. GS is generally well tolerated, and does not appear to affect glucose (blood sugar) metabolism adversely.
Chondroitin sulfate (CS). CS was significantly more effective than placebo at reducing pain and improving function in several double-blind trials. Results were typically assessed after 3 months. CS has anti-inflammatory activity, and X-rays taken after 1 year of treatment suggested that CS may prevent or delay the progression of osteoarthritis (double-blind study).
MSM – Methylsulfonylmethane is a type of sulphur compound that is naturally present in the body (i.e. it is a form of sulfur). Several studies performed in the late 1990’s have revealed that MSM does have a favourable effect and assists in rebuilding worn or damaged cartilage.
Vitamin E – Twenty-nine patients with OA at various sites were randomly assigned to receive (single blind) 600 mg of vitamin E (type not specified) per day or a placebo for ten days, and then the alternate treatment for an additional ten days.27 Fifty-two percent of the patients reported a reduction in pain while receiving vitamin E, compared with only 4 percent receiving placebo (p < 0.01). In another study, 53 patients with OA of the hip or knee were treated for three weeks with vitamin E (d-alpha-tocopheryl acetate 400 mg three times per day; equivalent to approximately 600 IU three times per day) or diclofenac (50 mg three times per day).28 Both treatments appeared to be equally effective in reducing the circumference of knee joints and walking time, and in increasing joint mobility.
Vitamin C. Useful to support connective-tissue metabolism: Epidemiological and uncontrolled studies suggest that vitamin C may be protective. I recommend my patients to take Vitamin-C.
Boron. Supplementation with 6 mg/day for 8 weeks resulted in symptomatic improvement in a small, double-blind trial. It is possible that boron supplementation is helpful only when dietary intake of boron (which is partly a function of soil content) is low. This is not uncommon in New Zealand, and may well hold true for many other countries where trace elements are low in the soil.
Omega 3. I always recommend a top quality Omega 3 product when a patient presents with OA. Research has recently shown that Omega 3 has anti inflammatory effects that may be helpful for arthritis sufferers. One important study showed beneficial effects when people took several capsules a day, though other research has suggested that benefits can be expected from taking only a few capsules daily. Omega 3 may help reduce the pain of osteoarthritis, according to researchers at Cardiff University. Omega-3 fatty acids in the oil appear to switch off the collagen-degrading enzymes that break down joint cartilage, slowing cartilage destruction and reducing inflammation, which lessens arthritic pain. Of the subjects who took 1,000 mg of Omega 3 supplements, 86% had absent or reduced levels of the degrading enzymes, compared to 26% of subjects who took placebo.
The 31 subjects in both groups followed the regimen for 10 to 12 weeks prior to total knee replacement surgery. This breakthrough is hugely significant because it demonstrates the efficacy of a dietary intake of Omega 3 in patients with osteoarthritis taken prior to their joint replacement surgery. The data suggests that Omega 3 has a dual mode of action, potentially slowing down the cartilage degeneration inherent in osteoarthritis and also reducing factors that cause pain and inflammation.”