Understanding Food Allergies and Intolerances
Many people come to me with questions about food allergies and intolerances. A common misconception is that all adverse reactions to food are allergies, when in fact, many are intolerances. So, how can you tell the difference?
Identifying Food Allergies vs. Food Intolerances
How do you know if you are actually allergic to a food or simply intolerant to it?
A food allergy is a specific type of adverse reaction mediated by the immune system. Adverse food reactions can manifest as any noticeable change in how we feel or function after consuming certain foods. Symptoms may include a rash, achy joints, or fatigue, among others.
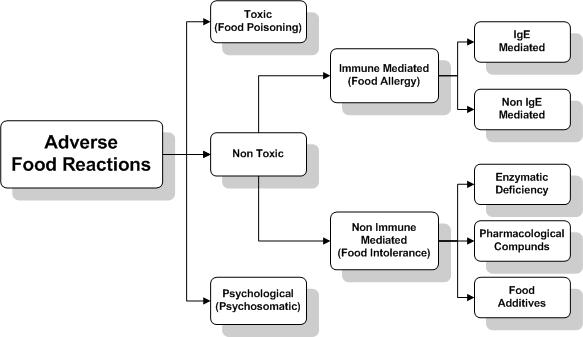
Adverse Food Reactions – Three Types
1. Toxic: Commonly known as food poisoning and results from contaminants in the food.
2. Psychological or Food Aversion: Related to a former ill experience and is psychosomatic.
3. Non-Toxic: Divided into two groups:
– Non-immune-mediated reactions (Food Intolerance): Can mimic allergic inflammation and may occur from food additives, pharmacological compounds, or enzymatic deficiency (i.e., lactose intolerance).
– Immune-mediated reactions (Food Allergies): Divided into IgE- and IgG (or non-IgE mediated) reactions.
Food Allergies
A true food allergy is not as common as you may think. Food intolerances are much more common in my experience. A food allergy is immune mediated and involves a reaction to a food or drink, which involves the immune system. We categorise food allergies into two groups: those which are more immediate (IgE immune response), and those which are more delayed (IgG immune response).
Let’s look at both:
– Immediate Food Allergy the Type 1 or IgE Response

Food allergies are immediate or delayed. With an immediate reaction, it will be quite noticeable and could take place within minutes to a few hours after ingestion of the offending substance. The best known and most studied form of food allergies is called a Type 1 immune reaction, or IgE mediated response. Type 1 food allergies occur in less than 5 percent of the population, mostly in children. They are also called “immediate onset” or “atopic” food allergies. These types of allergies usually occur in the genetically predisposed individual.
 The RAST Skin Prick Test
The RAST Skin Prick Test
Since this pathway occurs immediately, it is very easy to recognize a Type 1 allergy as a problem after an exposure to the irritant. This is the immunological pathway behind seasonal allergies, such as hay fever. The most common test for this type of reaction is the “scratch” or “RAST” test, which involves scratching the skin and applying a test substance and then waiting for a “wheal and flare response”, often a skin reaction.
Type 1 Food Allergy Symptoms
 The allergen and resulting symptoms are unique to the individual affected. Symptoms can be very individual. Some people don’t have any idea that they have food allergies.
The allergen and resulting symptoms are unique to the individual affected. Symptoms can be very individual. Some people don’t have any idea that they have food allergies.
Once the potentially allergenic foods become digested, broken down protein particles enter the bloodstream. The body rejects some of these food nutrients or other food components because of the immune system’s response. The immune system produces antibodies and other related elements that fight the protein particles. And that’s when the symptoms start.
Not long after the response, allergy symptoms become apparent, sometimes including swollen hands, itchy and swollen eyes, sensations of the lungs, and, if acute, even the closing of the larynx or throat. Anaphylaxis is the most alarming response. It means you can’t breathe; you have a fast heart rate, and there could be feelings of panic. Other symptoms may include stomach cramping, diarrhoea, hives, swelling, itching and various skin rashes.
Immediate Food Allergy (IgE) Summary
- – We call these the “Type One” toxic immune reactions, and they are quite obvious.
– At most, only 1 or 2 foods (rarely more) are involved in causing these allergic symptoms.
– Small, even the tiniest trace amounts of food can trigger these intense allergic reactions, including anaphylaxis.
– Allergic symptoms commonly appear 2 hours or fewer after consumption of offending foods.
– Primarily affects the skin, airway and digestive tract manifesting in “classical” allergies such as asthma, rhinitis, urticaria, angioedema, eczema, vomiting, diarrhea and anaphylaxis.
– Common in children, these reactions do occur in adults, albeit less commonly than the delayed (IgG) allergies.
– Some experts claim that addictive cravings and withdrawal symptoms are rare to nonexistent in children with IgE allergies.
– Except for infants and young children, the offending food is commonly self-diagnosed.
– Allergic food is rarely eaten.
– Commonly a permanent, fixed food allergy, but sometimes these allergies can become mild or even disappear entirely.
– Frequently, IgE “RAST” positive and skin test positive, but not necessarily so.
reactions can occur (e.g., eczema), the IgG antibody is not characteristically involved in IgE responses. - Mast cells, basophils, histamine and tryptase release are all commonly involved in this type of reaction.
– Delayed Food Allergies – Type 3 or IgG Response
 Non-IgE-mediated allergies involve antibodies other than IgE (e.g.: IgG). Symptoms of an IgG-dependent reaction may occur hours to days following exposure to the allergen. When foods are involved, we often refer to these as “delayed food reactions”.
Non-IgE-mediated allergies involve antibodies other than IgE (e.g.: IgG). Symptoms of an IgG-dependent reaction may occur hours to days following exposure to the allergen. When foods are involved, we often refer to these as “delayed food reactions”.
Much more complex mechanisms are involved in the delayed response. Here, the IgG antibody will bind to the food antigen and form an immune complex. An immune complex, sometimes called an antigen-antibody complex or antigen-bound antibody, is a molecule formed from the binding of multiple antigens to antibodies. The bound antigen and antibody act as a single object, effectively becoming an antigen of its own. Let’s leave it at that, or I’ll lose too many readers…
What happens to these “complexes”, is that they travel in the bloodstream throughout the body. They eventually deposited in various tissues and trigger inflammatory reactions. It is most unfortunate, but conventional medicine does not really recognise these types of immune responses.
According to the American Academy of Allergy, Asthma & Immunology (AAAAI), IgG food allergy testing test has “never been scientifically proven to accomplish what it reports doing” and “the scientific studies to support the use of this test are out of date, in non-reputable journals.” A 2016 study of IgG and food allergies, however, reports a different narrative. But because it was from the Annals of Saudi Medicine (ASM), they perhaps viewed it as “non-reputable” science. Rather sad.
Delayed Food Allergy (IgG) – Summary
– These delayed food reactions are not immediate, making them almost impossible to detect without sophisticated blood testing.
– More allergic responses typically occur here, with anywhere from 3 to 10 food allergens, sometimes even up to 20 foods.
– Larger amounts of food and multiple feedings are often required to provoke these types of allergic reactions.
– Allergic symptoms commonly appear 2 to 24 hours after consuming the offending foods, but symptoms often appear 48 to 72 hours later.
– Any tissue, organ, or system of the human body can be affected.
– Very common in children and adults, with over 50 medical conditions and 200 symptoms provoked, worsened, or caused by IgG allergic reactions to foods.
– Addictive cravings and withdrawal symptoms can be clinically significant in 20 to 30% of patients.
– Because of multiple foods and delayed onset of symptoms, the offending foods are rarely self-diagnosed.
– Allergic foods are commonly favorite foods, frequently eaten, and eaten in larger amounts.
– Allergy to foods is commonly reversible.
– Skin test negative, IgE “RAST” negative.
– IgG ELISA (Type II) positive; IgG food immune complex (Type III) and/or cellular (Type IV) reactions may be involved as well.
Food Allergies: What To Do
 The Hypo-Allergenic Diet FREE Handout
The Hypo-Allergenic Diet FREE Handout
Major allergens may include eggs, dairy, gluten or wheat, corn, peanuts, shellfish, fish, oranges, bananas, and chocolate. Our Hypo-Allergenic Diet Sheet – downloadable here, provides good indications of the most and least allergenic foods.
Babies and Food Allergies
 IIt is striking how many women come to my clinic with a child covered in eczema. Eczema can cover the child in a red, itchy rash and be miserable. Often, the child has been placed on a cow’s milk formula after having been breastfed for a few weeks, which can be too young to be introduced to cow’s milk protein. By utilizing the Hypo-Allergenic Diet and dramatically improving the mother’s diet (if the child is being breastfed), you can help your child overcome eczema.
IIt is striking how many women come to my clinic with a child covered in eczema. Eczema can cover the child in a red, itchy rash and be miserable. Often, the child has been placed on a cow’s milk formula after having been breastfed for a few weeks, which can be too young to be introduced to cow’s milk protein. By utilizing the Hypo-Allergenic Diet and dramatically improving the mother’s diet (if the child is being breastfed), you can help your child overcome eczema.
Keep An Open Mind!
Always keep an open mind and use common sense with your healthcare practitioner. If they are dogmatic and refuse to believe that you are interested in your treatment options, both conventional and natural, it may be time to move on. Minds are like parachutes; they function best when they are open.
References
- S. Leng, J. McElhaney, J. Walston, D. Xie, N. Fedarko, G. Kuchel (October 2008). “Elisa and Multiplex Technologies for Cytokine Measurement in Inflammation and Ageing Research”. J Gerontol a Biol Sci Med Sci 63 (8): 879–884. PMID18772478.
- M. Adler, S. Schulz, M. Spengler (2009) Cytokine Quantification in Drug Development: A comparison of sensitive immunoassay platforms. Chimera Biotech. (Report). Retrieved 26 January 2010.
- MedLinePlus. “HIV ELISA/western blot.” U.S. National Library of Medicine. Last accessed April 16, 2007. http://www.nlm.nih.gov/medlineplus/ency/article/003538.htm
- U. S. Food and Drug Administration. “Food Allergen Partnership.” Last accessed April 16, 2007. http://web.archive.org/web/20080325193553/www.cfsan.fda.gov/~dms/alrgpart.html
- YALOW R, BERSON S (1960). “Immunoassay of endogenous plasma insulin in man”. J. Clin. Invest. 39: 1157–75. doi:10.1172/JCI104130. PMID 13846364.
- Lequin R (2005). “Enzyme immunoassay (EIA)/enzyme-linked immunosorbent assay (ELISA).”. Clin. Chem. 51 (12): 2415–8. doi:10.1373/clinchem.2005.051532. PMID 16179424.
- Wide L, Porath J. Radioimmunoassay of proteins with the use of Sephadex-coupled antibodies. Biochem Biophys Acta 1966;30:257-260.
- Engvall E, Perlman P (1971). “Enzyme-linked immunosorbent assay (ELISA). Quantitative assay of immunoglobulin G”. Immunochemistry 8 (9): 871–4. doi:10.1016/0019-2791(71)90454-X. PMID 5135623.
- Van Weemen BK, Schuurs AH (1971). “Immunoassay using antigen-enzyme conjugates.”. FEBS Letters 15 (3): 232–6. doi:10.1016/0014-5793(71)80319-8. PMID 11945853..


 The RAST Skin Prick Test
The RAST Skin Prick Test The Hypo-Allergenic Diet FREE Handout
The Hypo-Allergenic Diet FREE Handout
Hello ~
Ten days ago I started the CanXida diet /cleanse and six days ago started with the Cleansing pills. For three days I took one pill daily, and then two pills daily for the last three days. I am following your suggested protocol and am excited to experience long term results.
I am experiencing facial skin rash that started surfacing two days ago… delayed food allergy to I believe is the garlic in the cleanse pills. I’ve battled symptoms for 10+ years and 2 years ago had to stop garlic intake as it created facial rash.Any suggestions on how to cope? As I keep taking the pills will the garlic ‘allergy’ dissipate? I’m assuming it will take quite awhile – months to a year?
Nine years ago, I eliminated the night shade vegetables, dairy and gluten from my diet , so my current diet is very limited. Is it possible to consult with someone on my challenges? Thanks a bunch!