Why do so many doctors get the skin infection diagnosis wrong? You'd be surprised how many, be sure to get the right diagnosis before considering medical creams and other pharmaceutical drugs for your skin condition.
Skin fungal infections can be tricky to identify and are often mistaken for conditions like eczema or psoriasis. As a practitioner, I’ve seen many patients in my clinic misdiagnosed with these conditions when they were actually dealing with a yeast skin infection. The itching, redness, and flaking skin caused by fungal infections can look similar to other types of dermatitis, making it easy to confuse the two. Unfortunately, it’s not uncommon for someone with eczema to also develop a fungal infection, which can further complicate the diagnosis.
The skin is our body’s largest organ and serves as a protective barrier. But when it’s compromised, whether by external factors or internal imbalances, it can become a breeding ground for fungal infections. Up to 15% of the world’s population is infected with dermatophytes, a group of fungi responsible for common infections like jock itch, athlete’s foot, and ringworm [oai_citation:1,Intestinal Candidiasis: Symptoms, causes, treatments, and your questions answered.] These fungi thrive in warm, moist areas of the body, such as the creases and folds of the skin, where they cause persistent itching and discomfort.
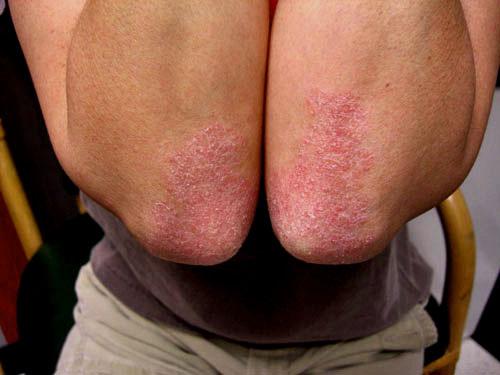
Fungal infections often cause symptoms like itching, redness, and flaking skin. These signs are particularly prevalent in the folds of the body, such as under the breasts, in the groin area, and between the toes. These symptoms can easily be mistaken for eczema or psoriasis, but with a bit of experience, you can learn to recognize the difference. Fungal infections typically thrive in warm, moist environments, so if a patient reports persistent itching and discomfort in these areas, it’s worth considering a fungal infection as a possible diagnosis.
Treating fungal skin infections involves more than just applying a topical cream. While antifungal creams can help alleviate symptoms, they often don’t address the underlying cause of the infection. In my experience, patients who receive only local treatments without addressing systemic factors often see their symptoms return. For more effective results, I recommend a combination of topical and systemic treatments, particularly for those with chronic or recurrent infections.
Preventing fungal infections involves taking steps to reduce moisture and warmth in susceptible areas. Wearing breathable clothing, keeping skin dry, and maintaining good hygiene are crucial. For those at higher risk, such as individuals with diabetes, it’s essential to monitor blood sugar levels and manage any underlying health conditions that could contribute to the infection.
It’s really important to get an accurate diagnosis if you suspect a fungal skin infection. While visual identification can be helpful, laboratory testing is often necessary to confirm the presence of a fungal infection. Pathology-based lab technicians can examine skin samples under a microscope to determine the exact type of fungus involved, ensuring that the treatment plan is tailored to the specific infection.