When your thyroid gland generates too much of the hormone thyroxine (T4), you have hyperthyroidism (overactive thyroid). Hyperthyroidism causes your body's metabolism to speed up, resulting in common symptoms such as unexpected weight loss, fast or irregular pulse, perspiration, and agitation. Hyperthyroidism may be treated in a variety of ways, and I'll be discussing both pharmaceutical drug options and look at natural medicine treatment as well.

When your thyroid gland generates too much of the hormone thyroxine (T4), you have hyperthyroidism (overactive thyroid). Hyperthyroidism causes your body’s metabolism to speed up, resulting in common symptoms such as unexpected weight loss, fast or irregular pulse, perspiration, and agitation. I will discuss both pharmaceutical drug options and examine natural medicine treatment as well for treating hyperthyroidism.
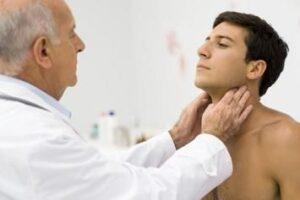
The thyroid gland, located below the Adam’s apple, produces thyroxine, essential for normal physical and mental development. Babies in New Zealand are screened for thyroid hormone deficiency at birth. In adults, thyroxine maintains the right metabolic rate. An overactive thyroid leads to hyperthyroidism, while an underactive thyroid causes hypothyroidism.
Goitre is the name given to a visible swelling of the thyroid gland in the neck. The goitre is usually normally active. That is, the thyroxine level in the blood is normal and the metabolic rate is normal. Most goitres cause no general symptoms and can often be ignored. Some people with a goitre may be advised to have simple diagnostic tests to find out exactly what kind of goitre it is and to test for the unlikely possibility of a low-grade cancer.
Fortunately cancer of the thyroid is very rare. When it does occur it is nearly always low grade, can be removed by surgery, and has a much better outlook than most other types of cancer.
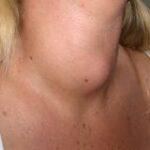
Treatment can easily resolve virtually all forms of thyroid disease, leading to good health. If left untreated, however, under-active or overactive glands can cause years of severe ill health or even death. After the initial assessment you may be as ked to return to the clinic for follow-up in conjunction with your own doctor.
 The hypothalamus is a part of your brain that helps connects the way you think and to your hormone system. This way, the way you think and feel on a minute to minute basis affects your hypothalamus, which in turn stimulates the pituitary gland.
The hypothalamus is a part of your brain that helps connects the way you think and to your hormone system. This way, the way you think and feel on a minute to minute basis affects your hypothalamus, which in turn stimulates the pituitary gland.
The pituitary is called the “master gland” or the conductor of the body’s hormonal orchestra. The walnut-sized gland is a lot like the sun in our universe, it is critical to ensure that life on earth is possible, nothing can live without that sun.
The pituitary is stimulated in turn by the hypothalamus to release TSH (thyroid stimulating hormone) that stimulates your thyroid into action. With clock-like accurate precision, the hormonal control of your hypothalamus – pituitary – thyroid feedback loop works 24/7. If you live in a low-grade stressful situation, your hypothalamus (your feelings and thoughts) will give your thyroid wrong messages, causing over-stimulation that eventually leads to hyperthyroidism or hypothyroidism.
 The most common form of hyperthyroidism results from unusual antibody levels circulating in the blood stream which stimulate the thyroid (Grave’s Disease). Over activity is not caused by stress or changes in the diet. It may wax and wane in an individual over a period of years. Women are more often affected than men and thyrotoxicosis may appear for the first time three to six months after pregnancy. There are several other potential causes of hyperthyroidism, apart from Graves’ disease, that include:
The most common form of hyperthyroidism results from unusual antibody levels circulating in the blood stream which stimulate the thyroid (Grave’s Disease). Over activity is not caused by stress or changes in the diet. It may wax and wane in an individual over a period of years. Women are more often affected than men and thyrotoxicosis may appear for the first time three to six months after pregnancy. There are several other potential causes of hyperthyroidism, apart from Graves’ disease, that include:
The exact cause of an overactive thyroid is unknown, but genetic predisposition and personality traits may play significant roles.
Hyperthyroidism can be inherited, and indeed it often is in many cases. The patient may well have had a mother, an aunt or a close or distant relation who had an overactive thyroid gland. Hyperthyroidism can occur for many reasons, and I wonder whether the over activity of the gland has caused the patient to become anxious, or whether the patient’s inherent anxiety caused the thyroid itself to become overactive.
Diagnosing hyperthyroidism can be challenging despite its prevalence, often overshadowed by hypothyroidism.
A study from 2019 concludes with “mental disorders, depression and anxiety often merge with Grave’s disease. Psychosocial factors including stress and disease awareness as well as biological factors including the effects of thyroid hormones may influence the course of a disease.”
It is surprising how many hyperthyroid patients we encounter in my clinic from time to time. There are plenty of these patients out there, but has anyone diagnosed them? When it comes to thyroid disorders, most of the attention focuses on the under-activity of this vitally important gland. But what about the many patients who have over-activity of the thyroid gland?
Clinical Symptoms and Impact
Hyperthyroidism affects different people in different ways. Many experience weight loss, despite increased appetite, tiredness, nervous symptoms and a dislike of hot weather. Shakiness of the hands and awareness of a rapid heart beat and difficulty sleeping are also common. Hyperthyroidism is a prolonged illness which, if untreated, can have severe consequences. Everyone who has it needs treatment, careful supervision is also required, usually for many years.
Personal Experience and Patient Care
 I’ve always spent time with hyperthyroid patients in the clinic, encouraging them to slow down. I advise them to take their time when walking, talking, exercising, eating, and going about daily life. This is quite difficult for the average hyperthyroid patient because they tend to see the world a little differently from you or me. My mother was hyperthyroid, and living with someone with this hyperactive condition helps you understand it and how anxiety drives the person. In her late 70s, my mother also suffered from osteoporosis, one of the symptoms of hyperthyroidism.
I’ve always spent time with hyperthyroid patients in the clinic, encouraging them to slow down. I advise them to take their time when walking, talking, exercising, eating, and going about daily life. This is quite difficult for the average hyperthyroid patient because they tend to see the world a little differently from you or me. My mother was hyperthyroid, and living with someone with this hyperactive condition helps you understand it and how anxiety drives the person. In her late 70s, my mother also suffered from osteoporosis, one of the symptoms of hyperthyroidism.
Some hyperthyroidism symptoms are outwardly visible, while others are subtle and difficult to detect at first. The following are some of the characteristic signs and symptoms of hyperthyroidism, according to the National Institutes of Health (NIH):
Here are some of the main points I’ve found in a person with an overactive thyroid gland. These signs and symptoms are some of the key ones I’ve observed with hyperthyroid patients over the years:
Impact on Daily Life and Productivity
 Sometimes when you are a hyperthyroid, your medical doctor may just see you as an anxious patient and give you some Xanax or Valium. Studies of hyperthyroid patients found that symptoms of anxiety and depression disappeared within months of starting anti-thyroid drug treatment, indicating that increased levels of thyroid hormones may contribute to anxiety and depression
Sometimes when you are a hyperthyroid, your medical doctor may just see you as an anxious patient and give you some Xanax or Valium. Studies of hyperthyroid patients found that symptoms of anxiety and depression disappeared within months of starting anti-thyroid drug treatment, indicating that increased levels of thyroid hormones may contribute to anxiety and depression
Personal Health Monitoring
If you identify well with the symptom list above, ensure you check your blood levels for hormones T4, T3, and TSH. If you notice any swellings in your neck or feel a lump in your throat, make sure you complete your thyroid antibody levels (blood test) as well.
Physicians who diagnose a disorder and prescribe a drug sometimes get it wrong, as well as patients who feel that they have a serious disease that needs treatment, but self-diagnose with Dr. Google before trying to convince their doctor likewise. I’ve seen both in my clinic. Hyperthyroidism can and is unfortunately regularly misinterpreted for anxiety disorder. I’ve seen many hyperthyroid patients over the years, and have come to recognise them.
A Google search for the topic “thyroid” on a few prominent medical websites will reveal misguided information when it comes to natural medicine, instilling confusion and even fear in those who chose to go to such websites:
I agree that while it is important and vital to control symptoms, to avoid complications and ensuing health problems, it is also important to think about incorporating other less invasive therapies beneficial for the thyroid patient, and to be wary of disease mongering online.
Unusual antibodies circulating in the bloodstream, which stimulate the thyroid, are believed to cause the common form of hyperthyroidism (Grave’s Disease). Despite claims that overactivity is not caused by stress or changes in diet, I have observed otherwise. Symptoms of Grave’s disease can fluctuate in severity over years. Women are more frequently affected than men, and thyrotoxicosis may first appear three to six months after pregnancy.
I have seen patients develop hyperthyroidism, and with a turnaround in diet and especially in lifestyle they became euthyroid again, meaning “well” thyroid. It has happened to several patients I’ve known, but it is not an easy task by any means, and there is no doubt that for some, drugs such as Carbimazole can be used effectively as a stop gap measure.
Hyperthyroidism affects different people in different ways. Many experience weight loss (despite increased appetite), tiredness, nervous symptoms and a dislike of hot weather. Shakiness of the hands, sweating (perspiration) and awareness of a rapid heart beat and difficulty sleeping are also common. Hyperthyroidism is a prolonged illness which, if untreated, can have severe consequences. Everyone who has it needs treatment. Careful supervision by a doctor is also required, usually for many years.
There are three different ways to treat an overactive thyroid:
Once the diagnosis is made, most people are given tablets such as Carbimazole. If you take them regularly, there is a marked improvement of symptoms in most people after three to four weeks. These tablets act as a brake on the thyroid by blocking an enzyme in the gland. In themselves the tablets don’t make the unknown cause of hyperthyroidism go away. But by taking the tablets for one or more years, the disorder may then disappear by itself as mysteriously as it came, just with the passage of time.
You will enjoy excellent health as long as you take the tablets and monitor the thyroxine level with a blood test. If you forget a dose you can ‘double-up’ with the next dose. Even after a year or more of treatment however, on stopping the tablets hyperthyroidism returns in nearly two thirds of patients, sometimes within weeks. In a minority, about one third, there may be no return of symptoms even for years.
When beginning treatment with antithyroid drugs, most people suffer no ill effects. Rarely (one in every thousand people), an important side effect may develop because of lowering of the white cell count in the blood. The symptoms of this side effect may include a sore throat, mouth ulcers or high fever and usually begin within two to six weeks of starting treatment. If you experience these effects while taking antithyroid tablets, you must contact your doctor immediately. Your doctor can arrange a measurement of your white blood count, and the effect is rapidly reversed by stopping treatment. Although this is a rare occurrence, it is important to stay alert for it.
About 3 percent of patients experience a more minor but irritating side effect: an itchy red skin rash that typically develops within two to six weeks of starting the tablets. While this rash may resolve on its own and allow continued tablet use, if it persists, patients should stop the pills and contact their doctor for further advice. Switching to an alternate drug is often possible. Antithyroid tablets, whether Carbimazole or PTU, can be safely taken under supervision during pregnancy and breastfeeding. Fortunately, an overactive thyroid often improves during pregnancy, only to recur 2 to 6 months after delivery.
My advice for most patients with more sever forms of hyperthyroidism is to stay on Carbimazole for some time until you are stable on the lower dosages. Many patients can eventually go onto a very low dose, and some can even discontinue here or there, although this should only be ever attempted under supervision!
My apologies for the oversight. Here it is in active voice:
Radio-iodine treatment is often recommended once doctors bring the overactive thyroid under control with tablets. The great advantage of radio-iodine is that doctors administer it at an outpatient visit as a single tasteless drink. It has little or no side effects but “smoothly and painlessly” “cures” the thyroid condition. Radio-iodine is the most common form of treatment worldwide and has been used for 50 years. I always caution patients when considering this toxic concoction, and in most cases, Carbimazole will hold the hyperthyroid condition at bay. If I have an extreme patient who cannot be controlled by Carbimazole or natural treatment recommendation, in some (I’ve only ever seen one in the twenty years I’ve treated patients) cases this extreme form of therapy may actually be required.
Naturally, none of us likes the idea of taking in radioactive substances unless it is absolutely necessary. Doctors will assure you that radio-iodine, when administered under their prescription, poses “no cause for alarm.” It targets the thyroid gland with concentrated radiation, minimizing exposure to other parts of the body. The majority of the radioactivity is excreted through urine.Glow in the dark you say. Because it is radioactive iodine, there are some precautions necessary in the first few days of treatment. Findings from a 2019 study of patients who received radioactive iodine (RAI) treatment for hyperthyroidism show an association between the dose of treatment and long-term risk of death from solid cancers, including breast cancer.
I beg to differ with the scientific opinion, and have helped many patients avoid drinking a radio-active solution, in favour of taking Carbimazole. In all the years I’ve seen patients, only one lady did not respond to Carbimazole and had to resort to the radioactive solution.
Naturally, none of us likes the idea of taking in radioactive substances unless it is absolutely necessary. In the case of radioiodine given under a doctor’s prescription, the choice is yours, you don’t have to take this option if you don’t want to, so speak up. The radiation dose you drink will become concentrated in the thyroid in order to “kill” it. Great, and because it is radioactive iodine, there are some precautions necessary in the first few days of treatment.
Radioactive iodine is certainly never given to pregnant women or children. Amazing, although doctors say this treatment is “safe”, and say the although there is no evidence of harm to family members, they still advise against “intimate or prolonged body contact for 2 to 4 days after treatment”. Babies and children in particular, are thought to be more sensitive to unnecessary exposure to radiation. Perhaps drinking something that is radioactive may not be all that safe?
The radioiodine does most of its work in destroying the activity of your thyroid gland over the first 4 to 6 weeks but continued benefits such as shrinkage and disappearance of the goitre continue for about 6 months. If you take Carbimazole tablets, your doctor will instruct you to stop them 5 days before therapy and restart them one week afterwards, continuing until your first follow-up visit. Typically, your doctor will require you to continue monitoring blood tests at 2-4 week intervals until the results stabilize. In about a quarter of individuals, a second radioiodine treatment may be necessary for a “complete cure”.
What they should tell you is this, that most who drink a radioactive drink will go on to develop – hypothyroidism, that’s right, an under active thyroid gland, and when this occurs you will be asked to take thyroxine tablets on a lifelong basis. Even if your thyroid gland function remains normal in the first year of treatment, a regular annual blood test of thyroid function is necessary indefinitely because an underactive thyroid can still happen many years after radioiodine treatment.
Radioactive iodine is not given to pregnant women. Although there is no evidence of harm to family members, doctors advise against intimate or prolonged body contact for 2 to 4 days after treatment. Babies and children in particular, are thought to be more sensitive to unnecessary exposure to radiation.
The nature and duration of precautions will depend on the recommended dose and your family or job circumstances. The clinic doctor will discuss and write down more specific precautions as they apply to you.
The radio-iodine does most of its work over the first 4 to 6 weeks but continued benefits such as shrinkage and disappearance of the goitre continue for about 6 months. IIf you take antithyroid tablets, your doctor will instruct you to stop them 5 days before therapy and restart them one week afterwards, continuing until your first follow-up visit. Typically, you will need to monitor blood tests at 2-4 week intervals until the results stabilize. In about a quarter of individuals, a second radioiodine treatment may be necessary for complete resolution.
An expected effect of treatment is that the thyroid gland may become under-active in as many as one half in the first year. If this occurs it will be necessary for you to take thyroxine tablets. This is a small inconvenience to ensure continued normal thyroid function but you will need to take thyroxine on a lifelong basis. You will also be discharged from the clinic to the care of your GP, who will provide a three-monthly prescription of thyroxine tablets and arrange occasional blood tests to ensure that your dose of thyroxine tablets is suitable.
Even if thyroid gland function remains normal in the first year of treatment, a regular annual blood test of thyroid function is necessary indefinitely because an underactive thyroid can still happen many years after radio-iodine treatment.
Here’s a revised version of the snippet with appropriate subheadings added:
Rarely, neither tablets nor radioiodine treatment is suitable, and thyroid surgery may be recommended. About three-quarters of the gland is removed. There are definite risks to surgery, and because of the safety and simplicity of radioiodine, operations are infrequent nowadays.
Surgery was the common and preferred option years ago. It was once very commonly performed, akin to tonsillectomies in the 1950s. Interestingly, the most common operation performed in New York in 1900 was to remove 12 inches from the lower part of the bowel (colon) due to a “disease called constipation”.
This structure helps to segment the information clearly, highlighting the evolution of treatment options and the considerations around surgery for hyperthyroidism.
 Does anybody remember British comedian Marty Feldman? You would probably have to be a baby boomer like me.
Does anybody remember British comedian Marty Feldman? You would probably have to be a baby boomer like me.
Marty suffered from Grave’s disease. It became his “trademark signature,” making many people laugh and earning him a fortune. If you watch one of Marty’s comedy clips on YouTube, you’ll notice moments where his behavior is overly excited. This showcases Grave’s disease at its peak.
If you’ve been diagnosed with Grave’s disease, slowing down and consciously being aware of your speed are crucial actions to take. Despite doctors saying it “makes no difference,” I disagree based on my experience with many Grave’s patients over the years.
Those diagnosed with Grave’s disease (hyperthyroidism) would do well to slow right down. I have found that in most instances, hyperthyroid patients tend to walk fast, talk fast and move quickly in general. By slowing down the rate of speech and movement, it is possible to “ease off” that accelerator pedal. A person with Grave’s disease is like a car that’s speeding out of control and the driver just keeps on stepping on that accelerator pedal. What the hyperthyroid does something, she really goes for it 100%, there are no half measures!
My mother was a typical Grave’s disease example here. When she painted her own house (at 74yrs of age) she would use a power sander and work for hours on end. Oh, did I forget to mention to you that many hyperthyroid patients can tend to be very independent and stubborn? They want to take control and do it their way often. This can mean they find it difficult to delegate and work too hard, overdoing things. This typically overworks the muscles and places a continual demand on the thyroid gland to continually (over) produce the thyroid hormones T4 and T3. This results in painful and at times even burning muscles. Slow down! Read: Coping With Stress
A good thing to do is to slow down your rate of speech. During a consultation, I once recorded a woman with Grave’s disease, and when I played the recording back, she was amazed at how fast she spoke. Do you talk very fast, or have found that people find it difficult to follow you in a conversation? It could be that you are talking too quickly, just s l o w down a little. By slowing your rate of speech consciously for some time it wil become a habit. This in turn will slow your mind, and ultimately help to slow that poor thyroid gland down too!
People with hyperthyroidism often move very quickly, whether rushing to answer the phone or navigating through crowded aisles. They find it challenging to relax and slow down in their daily activities. If you tend to move quickly, try walking in waist-deep water in a swimming pool to slow down. Becoming consciously aware of your speed when exiting your car, answering the phone, or exercising can help you notice and adjust your rapid pace. Practicing this awareness can turn slowing down into a habit. You might also find it helpful to imagine observing yourself from an outside perspective or to have a friend or family member provide feedback over a few days. This feedback aims to support your health and well-being without criticism.
Some websites and books I have found tell you to avoid certain vegetables, claiming they can “exacerbate hyperthyroidism”, and that the natural treatment of hyperthyroidism includes avoiding such vegetables. These foods include rapeseed (used to make canola oil); the Brassica vegetables (cabbage, Brussel sprouts, broccoli, Chinese vegetables such as Bok choy, etc, and cauliflower), all which contain natural goitrogens, chemicals that cause the thyroid gland to enlarge by interfering with thyroid hormone synthesis. Read: Healthy Eating
I have found that actually including these foods in the diet can be favourable, as they inhibit and suppress thyroid hormone production. Other goitrogens include maize, kumara (sweet potato), lima beans, soy and pearl millet.
Even though no evidence proves these foods cause hyperthyroidism, some doctors still advise patients to avoid these foods in the natural treatment of hyperthyroidism.
In my opinion, it is actually worth having them in your diet for several months and gauge for yourself how your hyperthyroidism is responding. You be the judge, because everybody is different and people all react differently with the foods they eat.
My grandmother had most of her thyroid gland removed, and my mother about half of her thyroid gland. I noticed a nodule on the right side of my thyroid gland when I was forty – which completely disappeared after taking iodine. I didn’t live in the 1950’s, if I had a thyroid issue then, the doctors would have almost certainly removed part if not all my thyroid gland like my predecessors.
If you do have hyperthyroidism, find the cause. Do you have anxiety? This is a frequent cause. Has your doctor spoken to you about stress and anxiety, why not? You’ll get significant benefit from cultivating your calmness.
References
Article written – November 2006 Last update – February 2022