All cells in the body receive nutrients and oxygen through the circulatory system (cardiovascular system). It is made up of the heart and the blood arteries that run throughout the body. The arteries convey blood out from the heart, while the veins return it.
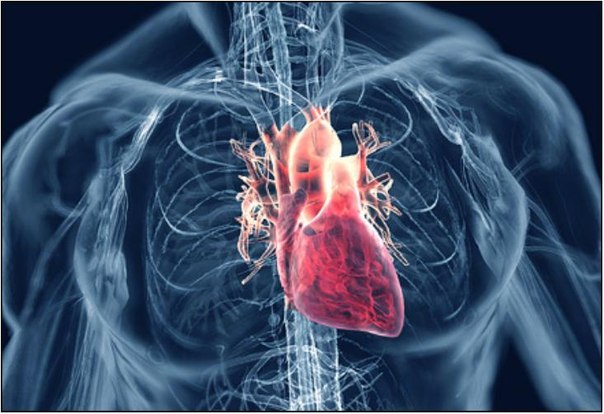
How Does Your Cardiovascular System Work?
In a nutshell, your circulatory system (cardiovascular system) transports oxygen-rich blood from the heart to the lungs. The heart then pumps oxygenated blood throughout the body via arteries. The veins return oxygen-depleted blood to the heart, where it is recirculated.
After your organs use up the oxygen they require and the nutrients you take in through your diet (that’s why you need to eat good foods) the blood has come to be depleted and has picked up any toxic residues and wastes such as carbon dioxide. Your circulatory system is literally a highway for nutrients and gases which are continually transported back and forth throughout your body.
This heart and circulatory system however is often the one which has the ability to cause you an incredible amount or grief as you age, and is reflected particularly in the high rates of circulatory disorders such as stroke and heart disease. One in four will die from heart disease who live in a developed nation, with one person dying every 36 seconds of heart disease in the USA.
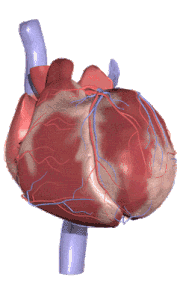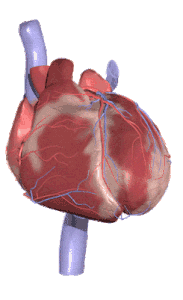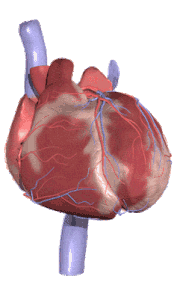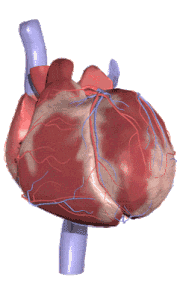 The heart is the main organ that pumps the blood back and forth throughout the body and does an incredible job of doing this, day in and out, beating thousands of times a day. Think of your heart as a muscular pump about the size of your fist which delivers vital oxygen and nutrients into all the cells of your body. This cone shaped powerful muscle has four chambers, and each of these chambers is connected by a series of one-way valves that let the blood flow in one side and then out the other.
The heart is the main organ that pumps the blood back and forth throughout the body and does an incredible job of doing this, day in and out, beating thousands of times a day. Think of your heart as a muscular pump about the size of your fist which delivers vital oxygen and nutrients into all the cells of your body. This cone shaped powerful muscle has four chambers, and each of these chambers is connected by a series of one-way valves that let the blood flow in one side and then out the other.
Blood which is spent of oxygen, or oxygen “poor” blood returns to the heart in the veins and collects in the right atrium and is then moved into the right ventricle which then pumps this de-oxygenated blood into your lungs for re-oxygenation.
Oxygenated blood then returns to the left atrium passing through the mitral valve and into the left ventricle. Blood is then pumped out with a lot of force (in a healthy heart) into the main artery of your body – the aorta. (see diagram) The blood (rich in oxygen) now travels through the aorta and several other arteries which branch off it into the body.
Most importantly, the oxygenated blood also travels through two coronary arteries to supply you heart itself with blood rich in oxygen. (see diagram). And it is these delicate arteries that are often implicated in a heart attack as they become clogged and affected by atherosclerosis. (plaqueing of the arteries).
Did you know that there are an estimated six thousand miles (almost 9,700 kilometres) of blood vessels which make up your circulatory system? The way I think of this system is like imagining a tree with its trunk, then branches and then the finer twigs, or a river with its many tributaries. The larger arteries branch into smaller arterioles and these in turn branch off into the tiniest of blood vessels called capillaries.
And it is these miniscule capillaries which end up feeding the cells of your body, supplying them with life-giving oxygen, removing the carbon dioxide as well as the cells waste products. The wastes and blood which is spent of oxygen are transported back to the heart in venules (small veins) and then into the larger veins and finally makes its journey all the way back to the right atrium.
This most elaborate system of pipes needs to be kept clear to accommodate the full force of contractions of your heart which permits an uninterrupted and strong blood flow. It is suffice to say that the walls of all these blood vessels needs to be (and stay) in top shape and free from any obstruction. The main thing to remember with your arteries is that the biggest focus is on high blood pressure, rather than issues with the veins. Veins do develop problems of their own, particularly with ageing, but it is the arteries we are most concerned about when it comes to high blood pressure.
You can read about the best blood tests to determine heart disease on this link, along with blood tests to evaluate heart health not commonly performed by mainstream medical doctors.