Eczema (also known as atopic dermatitis) is a skin condition that causes dry, red, itchy, and rough skin. It's one of numerous varieties of dermatitis. The skin barrier function is damaged by eczema. Because of the lack of barrier function, your skin becomes more sensitive and susceptible to infection and dryness.
 Eczema (also known as atopic dermatitis) is a skin condition that causes dry, red, itchy, and rough skin. It’s one of numerous varieties of dermatitis. The skin barrier function is damaged by eczema. Because of the lack of barrier function, your skin becomes more sensitive and susceptible to infection and dryness. Eczema is not harmful to health, it doesn’t mean your skin is dirty or sick, but it can be very uncomfortable and painful, especially when children are affected. There are many different treatments available, both medical and natural to assist you manage your symptoms.
Eczema (also known as atopic dermatitis) is a skin condition that causes dry, red, itchy, and rough skin. It’s one of numerous varieties of dermatitis. The skin barrier function is damaged by eczema. Because of the lack of barrier function, your skin becomes more sensitive and susceptible to infection and dryness. Eczema is not harmful to health, it doesn’t mean your skin is dirty or sick, but it can be very uncomfortable and painful, especially when children are affected. There are many different treatments available, both medical and natural to assist you manage your symptoms.
The term eczema is a word which comes from the Greek and when translated essentially means boil out. A long time ago health-care practitioners literally believed that if a person had eczema their skin was boiling, and that this outward manifestation was due to heat being produced in the body and eczema was the skin literally boiling out of the body.
About 1%-2% of adults have a skin rash which is due to eczema, and this skin condition is even more common in children. Most of those who are affected with eczema as adults will have their first episode before 5 years of age. For most eczema sufferers, this annoying skin disease will improve with time, but unfortunately for an unlucky few, eczema can be a chronic and recurrent disorder.
I’ve discovered that many health care professionals get confused with skin diagnoses, and various cases of psoriasis I have seen were diagnosed as eczema, and cases of dermatitis were diagnosed as eczema or psoriasis. A study conducted in 2020 found that ” a large percentage of misdiagnoses of common cutaneous (skin) diseases may be due to general paediatricians being undereducated in the field of dermatology”.
It can get very confusing indeed, but once you have seen countless skin cases you soon get a feel for what represents eczema and what is psoriasis or contact dermatitis. The term “dermatitis” is often given to skin cases which are inflammatory by nature, and hence eczema is sometimes called dermatitis for that reason. Here’s a good tip to remember in medicine, anything ending in “itis” generally refers to an inflammatory condition.
Doctors sometimes refer to eczema as “the itch that produces skin rashes.” Eczema can be extremely distressing for some children, and the rash can cause equally as much much distress for the parents because their child may even find it hard to get to sleep. Eczema will often become more more irritable as the skin warms up (in bed) which will make a child itch and scratch her skin until it literally bleeds.
I can usually identify eczema quite quickly just by looking at the rash and asking the patient (or caregiver) questions about how it appeared.
The four key elements in identifying eczema are:
Dyshidrotic eczema is a skin condition that develops as a sudden rash of small, itchy blisters on your palms and along the sides of fingers. Dyshidrotic eczema can also make blisters pop up on your toes and even on the soles of your feet. Treatment to clear up the blisters and relieve itching most commonly includes creams and ointments to rub on the affected areas.
The difference between dermatitis & eczema is not always that easy to determine both of these skin conditions are very similar. Dermatitis tends to be a more localised allergic reaction to a specific substance like a chemical in soaps or makeup, that comes in contact with the skin. Eczema differs from dermatitis in that it is often the result of an allergy, asthma or hay fever.
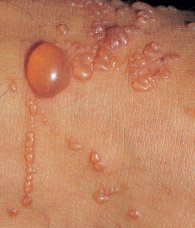
Dermatitis can be either acute or chronic, and in the acute skin lesions of dermatitis you will generally find small fluid-filled structures called vesicles that are usually found on red and swollen skin (see the image on the left). Dermatitis lesions can even resemble the vesicles of herpes at times and I have know this to confuse some practitioners.
When these little vesicles break open (and they can they can be so very itchy), fluid leaks out which will generally cause weeping and oozing to occur. When this fluid dries out, it produces a thin crust. In more chronic cases of dermatitis, you will find older lesions, and these vesicles may be harder to diagnose because they won’t have the characteristic fluid filled vesicles. A skin specialist can do an examination of the skin tissue under the microscope which will usually confirm the diagnosis.
I find that eczema differs from dermatitis in that it tends to run more in families (genetic) and can be a chronic ongoing condition. The eczematous lesions can and more likely with young children, become infected due to scratching, and like dermatitis, the eczema can crack, causing oozing and weeping of the area.
Your doctor with any infection may prescribe an antibiotic, further undermining the immune system and particularly the digestive system, causing leaky gut syndrome to develop. And unfortunately, leaky gut syndrome is linked to food allergies, which only further exacerbate the eczema.
My recommendations? Use Tea Tree oil on the skin with any infections, that will solve the problem quickly in most all cases. I’ve given up counting how many children I’ve seen who have developed recurring eczema after antibiotics. Ask any naturopath and they will be quick to tell you of the relationship of eczema and antibiotics and a child.
It is easy to get confused, some doctors even got both skin diseases mixed up.
If you want to know a lot more about psoriasis, the signs and symptoms and causes and my treatment recommendations for psoriasis then please go to our psoriasis page. Psoriasis is known as an auto-immune condition, meaning that it is caused by the immune system itself attacking the skin cells and causing certain cells to grow and multiply too quickly. It is quite different from eczema and dermatitis, and it is truely amazing how practitioners get skin conditions mixed up.
Atopy refers to a lifelong and inherited (genetic) predisposition to inhalant allergies such as asthma and allergic rhinitis (hay fever). While atopic eczema is not in itself an allergic disease, atopic patients are much more likely to have asthma, hay fever, and even various forms of dermatitis. Atopy is not as common as eczema itself, and can affect all races and ages, and particularly including young infants.

Here is a case of a 5 month old boy brought to our rooms with eczema and many other chronic health complaints, Anna, the boy’s mother, wrote a nice email which I have included below. “The biggest hurdle I have found in the dealing with my child’s allergies is the resistance of the medical system with anything natural, doctors were of no help at all”. Anna Reeves
“My name is Anna Reeves, and I don’t know if you remember, but I came to see you in August 2006 with my 5-month-old son Hamlin, who was exclusively breastfed and suffering from eczema, runny stools, excessive wind, sinus/breathing/ear problems, and reflux.
I saw you for an initial consultation, and you gave me dietary tips and a diet plan to follow (you suggested the most likely foods to be, etc). I also bought some children’s nutritional supplements from you. I started the diet that day and within literally two weeks the reflux/vomiting after feeding had stopped.
The eczema got worse and worse, though I knew I was doing the right thing (you said this may happen and explained why, which I found really helpful) and I persevered with the dietary changes you suggested. I didn’t use any steroid doctor-prescribed creams (only natural products to help soothe the skin)
Within 6 months Hamlin was ONE HUNDRED PERCENT symptom-free. It was truly unbelievable. Hamlin is now a healthy, happy, still completely symptom-free 17 month old. I am still breastfeeding and neither of us eat the allergenic foods you pointed out.
He is off the charts for his age in weight, and eats like a horse – meat, fish, seafood, vegetables, fruit and some gluten-free bread/pasta. I have learnt to cook and enjoy food around his allergies and realised that I was highly allergic to these foods myself, I can not tolerate them whatsoever. My own health and vitality has improved ten-fold.
Hamlin has had no immunisations (you advised me to think carefully about my choices in view of his allergies and poor immune function) I did further research and made a (informed choice as you pointed out) decision to not immunise. And my son has never been sick since I made the changes you suggested, nor needed to see any doctor or have any kind.
The biggest hurdle I have found, in the dealing with Hamlin’s allergy journey, is the resistance of the medical system – I found that doctors were no help at all. Most health care professionals attitudes as well, everyone I spoke with about my son’s eczema could only offer me interventions, like special formulas, herbs, steroid creams, etc. There was little support or understanding out there for self-management or alternative ways of dealing with allergies and actually getting to the bottom of the cause.
So, I am emailing you to share my story’s conclusion. I never thanked you and want to do so wholeheartedly. The consultations I had with you really gave me the tools to educate myself and free my son from our own personal hell due to the symptoms he and I, unknowingly, were suffering. I am so grateful that on a “desperate whim” decided to see you and you were there to share your knowledge.
You were understanding, easy to talk to and explained everything so well. I hope my story helps other parents seek help – like the information you gave me.
|
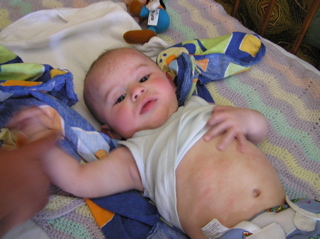
Hamlin (below) at 5 months
Hamlin (right) at 16 months |
 |
I have emailed you a photo of him at 5 months (to be honest I didn’t take any pictures when it got worse, I couldn’t bare to) – you can see the eczema on his cheeks, head and stomach. And another at 16 months. Please feel free to share these pictures with other mums so that they can see that there IS life beyond drugs and steroids.
Sorry this has been so long and please feel free to use any of it, in any way you see fit as a testimonial.
Thanks again Eric, for all your help”.
Anna Reeves New Zealand
It is generally agreed that the tendency towards atopy is a genetically inherited condition. I have found quite often that when a parent brings their child into our clinic with eczema, there is often a close relation such as the mother or father who also had eczema, or hay-fever or asthma as a child. People with eczema have been found to have a wide variety of abnormal immunologic findings which are probably related to one or more genetic defect. For example, such individuals tend to have elevated IgE antibody (immunoglobulin E) levels and may have issues in fighting off certain viral, bacterial, and fungal infections. Others will have a more exaggerated response towards certain triggers such as house dust or dust mites. People with eczema however may have elevated IgE and IgG levels, immediate or delayed immunoglobulins.
There is little doubt, like most other non-infectious diseases, eczema can be triggered by various environmental factors. One of the biggest finding I have seen with most all cases of eczema is excessive skin dryness, which seems to be due a lack of certain skin proteins. Any factor that promotes dryness is likely to exacerbate eczema.
The priority of the naturopath is to uncover the likely cause of chronic or acute conditions. Sometimes the cause is not always that apparent though. What if a child presents with eczema, and no parents, relations or any distant relatives have immune problems? Why would a child develop eczema? Surely there must be one or more causes why a child develops a skin condition such as eczema. There sure is, and in my opinion there are several likely reasons and here are a few likely causes which I see time and again in my clinic. One of the biggest reasons? – Antibiotics.
 Pharmaceutical Drugs Can Cause Eczema
Pharmaceutical Drugs Can Cause EczemaPharmaceutical drugs most common for producing eczema include: ALL antibacterial drugs (especially aminoglycosides, antibiotics like amoxycillin, ampicillin, erythromycin, gentamycin, lincomycin, rifamycin, cephalosporins), antimycotic (antifungal) drugs, anti viral drugs, tromantadine hydrochloride, idoxuridine, acyclovir (Zovirax), antiparasitic drugs, antihistamines, phenothiazines, steroids, non steroidal anti inflammatory drugs, anesthetics, and anticancer drugs. See: Drug Induced Dermatitis. See: Drug Rashes.
Ref: Drs Ruggero Caputo and Stefano Veraldi, two Italian dermatologists at the University of Milan (Eczema, Ronald Marks, ed., Martin Dunitz Ltd, London)
Eczema has many different causes, and there are several possible environmental causes apart from genetic and iatrogenic (drug-induced) causes I have already listed, here are the most common environmental causes of eczema.
 Your medical practitioner will generally prescribe a hydrocortisone cream which is generally regarded sufficient to “control” the rash. Once your doctor has diagnosed eczema, the mainstay of therapy is generally an anti-inflammatory medication and relief from the itching. Emolients (skin moisturisers ) are recommended to soften and moisten dried skin. What I find interesting is that medical professionals don’t generally consider the diet to be of much concern, and are quick to recommend a steroid cream to “cure” (more likely suppress) the rash of eczema. Apart from that, it is all about treatment rather than trying to establish any likely cause.
Your medical practitioner will generally prescribe a hydrocortisone cream which is generally regarded sufficient to “control” the rash. Once your doctor has diagnosed eczema, the mainstay of therapy is generally an anti-inflammatory medication and relief from the itching. Emolients (skin moisturisers ) are recommended to soften and moisten dried skin. What I find interesting is that medical professionals don’t generally consider the diet to be of much concern, and are quick to recommend a steroid cream to “cure” (more likely suppress) the rash of eczema. Apart from that, it is all about treatment rather than trying to establish any likely cause.
The other interesting point worth raising is that Western medicine has little if any regard for the digestive system’s involvement in terms of a person’s immune system. Natural health and integrative medicine practitioners are well aware of leaky gut syndrome, a condition where the small intestine becomes more permeable to the immune system, allowing certain protein molecules to adversely affect immunity. Antibiotic drugs are linked with destroying the beneficial as well as non-beneficial bowel flora, increasing bowel permeability, thereby facilitating the progress of leaky gut syndrome.
Prescription-strength steroid creams, moisturisers and sometimes antihistamine medications are the basic treatments offered. If your doctor has determined that you have a secondary bacterial infection complicating your eczema rash, then an antibiotic may be prescribed. For severe cases of eczema which do not respond to a high-potency steroid cream, alternate treatments with other aids may be tried, and these include coal tar, PUVA (psoralen + ultraviolet A light), and (heavens forbid!) if the case is particularly resistant to treatment, then chemotherapeutic drugs may even be prescribed – yes, for eczema.
In a few rare cases, eczema can become a systemic infection, the skin may become that irritated that it actually begins to breaks down and large areas can become infected. So what do you need to look out for? – If the rash has become red, hot, and very painful or if a fever develops, an emergency department visit may be necessary if you cannot see your doctor within 24 hours.
References:
Love the article!Learned sooo much than you!!! Where can I find the Hypo Allergenic Diet?
Where can I find the Hypo Allergenic Diet?
Hi there, just follow this link: https://ericbakker.com/article/food-allergy-and-food-intolerance/
Go to that page, and you’ll find a link to click called Hypoallergenic Diet