Vitamin D is a group of fat-soluble chemicals that increases calcium, magnesium, and phosphate absorption in the intestine, among other biological effects. Vitamin D3 and vitamin D2 are the most important molecules in this category in humans.

Vitamin D is a fat-soluble vitamin that is known as the “sunshine vitamin”. Unlike many vitamins, Vitamin D is naturally present in only a very few foods such as deep sea fish (liver), sardines, shrimp (prawns), eggs and fortified milk. This all important vitamin is added to others and available as a dietary supplement. It is also produced inside your body when ultraviolet rays from sunlight strike your skin and trigger vitamin D synthesis.
Are you outside enough to get the Vitamin D levels you require? There are a few big reasons and several smaller ones why you need to know about this amazing vitamin, which is also viewed as a hormone by some experts in nutritional medicine.
Most people don’t really know much about the remarkable actions of Vitamin D, it certainly is not just a vitamin necessary for producing strong bones. In fact, nutritional experts are continually learning more and more about this remarkable vitamin. Vitamin D produces multiple effects, including the repair and maintenance of each and every cell, as well as having the complex action of a steroid hormone that serves multiple gene-regulatory functions in your body. No other vitamin to this date has found to have such a complexity of action in your body. Is it any wonder we are starting to place an increasing amount of importance in the amazing vitamin?
Vitamin D helps to regulate many genes inside your body’s countless cells and your body’s complex DNA is activated by Vitamin D. Now you can understand why the vitamin which has so many different functions on so many different tissues of your body can have such a profound affect on a large number of health conditions and diseases. So far, scientists have found over 3,000 genes which are regulated by vitamin D. Nearly every single cell in your body from your head to your toe contain receptors which respond to Vitamin D.
Perhaps in the area of cancer is where most of the interest in Vitamin D remains at present, because research has discovered that Vitamin D can help you to prevent as many as 16 different types of cancer as well as reduce your risk of numerous chronic degenerative illnesses.
There has been a renewed interest in Vitamin D, and the interesting thing I find about Vitamin D is the amount of attention it has been given only the past few years or so and this is because of its connection with immunity and in particular with cancer. An increased cancer risk has been now positively linked with Vitamin D deficiency, and there is ample cancer in Australia and New Zealand for you to pay particular attention to this kind of research.
You would think because of the high sunlight levels in Australia and New Zealand that deficiencies of this vitamin would be uncommon, but this is clearly not the case. If a person lacks vitamin D, they have not only a higher chance of getting rickets and having soft bones, but are also more likely to get cancer and have an increased tendency to develop any one of several chronic diseases.
Deficiencies in vitamin D result in rickets in children and osteomalacia (soft bones) in adults. Both diseases are characterised by a softening of the bones caused by low amounts of calcium and phosphorous. Vitamin D deficiency also increases the risk for hip fractures in post-menopausal women, and is associated with a higher risk for breast cancer, especially in older women, and prostate cancer. There has been some concern that under-exposure to sunlight in older people, particularly if they live in northern regions, may put them at risk for low levels of vitamin D. A 1998 study suggests that vitamin D deficiency may be a significant problem in the general US population, even among younger adults. Experts note that adults may need higher daily amounts than the RDA suggests. Exposure to sunlight for about 15 to 20 minutes at mid-morning or mid-afternoon three times a week is also recommended for most people who live in temperate climates.
Vitamin D deficiencies are becoming much more common today with people spending more time inside and consuming fewer foods containing sufficient amounts of Vitamin D. Children in particular have been shown to have insufficient Vitamin D. Children in New Zealand Lacking in Vitamin D.
I frequently tell patients that in the old days (1940’s to 1960’s) people were inclined to eat more of the organ meats (liver, kidneys, etc) of an animal which contained a much higher amount of the fat soluble vitamins such as Vitamin D than they do today. Today, humans consume mainly the muscle meats and refrain from any “unclean” parts of an animal. In the years gone by it was not unheard of to eat the cartilage and even bone marrow of the animal. Is it any wonder that today we see so many nutritional deficiencies? Primitive tribes still eat most of an animal they kill, and have done so since time immemorial. Today, in the 21st century, we like everything clean, neat and sanitised, including our food.
 Who May Need Extra Vitamin D to Prevent a Deficiency?
Who May Need Extra Vitamin D to Prevent a Deficiency?Many people older than 50 are thought to have a higher risk of developing vitamin D deficiency. The ability of skin to convert vitamin D to its active form decreases with age, and the kidneys (which help convert vitamin D to its active form) have a tendency to reduce in function on average 1 – 2% per year after a person turns about 50. Children need careful Vitamin D assessment like adults, but are often overlooked as far as Vitamin D testing is concerned at the doctor’s clinic.
Do you have a fair skinned and red haired child who you protect from the sun, and cover in sunscreen vigorously with the slightest possibility of sunburn? I’d recommend a Vitamin D test for your child, and especially with those who do not spend enough time outside in the sun. The message about “Don’t let you child ever get sunburned” on TV reinforces a parent’s belief that the sun is evil and needs to be avoided. Those who drink plenty of alcohol are best to supplement with D3, but best to check your blood levels first as usual.
There is no doubt, it is very important for those who spend lots of time inside to go out and get sunshine very regularly, preferably every day. If it is not possible to get as much sunlight exposure as you should, then it becomes very important for individuals with limited sun exposure to include good sources of vitamin D in their diet. People living in southern latitudes such as the South Island of NZ, or women who cover their body for religious reasons, and people working in occupations that prevent exposure to sunlight like computer or retail based environments are all at a higher risk of Vitamin D deficiency. If you are unable to meet your daily dietary need for Vitamin D, they may need to supplement with a quality Vitamin D3 supplement.
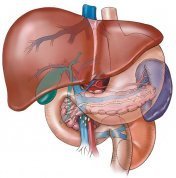 Vitamin D supplementation for those with fat absorption problems
Vitamin D supplementation for those with fat absorption problemsIndividuals who have reduced ability to absorb dietary fat (fat mal-absorption) may need extra vitamin D because it is a fat soluble vitamin. Some causes of fat mal-absorption are pancreatic enzyme deficiency, Crohn’s disease, gallbladder dysfunction, cystic fibrosis, celiac disease, liver disease, surgical removal of part or all of the stomach, and small bowel disease.
Symptoms of fat mal-absorption include diarrhoea and greasy stools. Excessive excretion of faecal fat is called steatorrhea, a condition that is suspected when the person has greasy, foul-smelling stool. Such stool may float on top of the toilet water and prove challenging to flush. Oil droplets may even be apparent in the toilet water following stool.
Those who have had their gallbladder removed are particularly at risk of a fat soluble vitamin deficiency. Make sure that you get your Vitamin D levels checked by way of a blood test a few months after you have had your gallbladder removed. In my experience, the D levels tend to be too low in many such cases.
Vitamin D supplements are often recommended for exclusively breast-fed infants because human milk may not contain adequate vitamin D. The American Institute of Medicine states that “With habitual small doses of sunshine breast or formula-fed infants do not require supplemental vitamin D.” Mothers of infants who are exclusively breastfed and have a limited sun exposure should be aware of increasing their infant’s sun exposure. Since infant formulae are routinely fortified with vitamin D, formula fed infants usually have adequate dietary intake of vitamin D.
A patient recently came to my room diagnosed with breast cancer. Her doctor told her that Vitamin D was “nonsensical” and had no effect on breast cancer whatsoever. Yet many studies now say the exact opposite. Worried about breast, bowel or prostate cancer? Have you Vitamin D blood levels checked – today.
A meta analysis (a whole lot of studies combined) has shown up to 70% or more risk reduction with breast cancer, bowel and prostate cancer. Is it any wonder that the drug companies and those who are involved in the cancer business are running scared? The Vitamin D blood test cost peanuts, pay for it privately if your doctor refuses to test you.
Vitamin D is a fat soluble vitamin which basically helps bones grow and form and is most beneficial for the immune system. To confuse you, in total there are 5 different D vitamins, form Vitamin D1 to Vitamin D5. The most common ones however are Vitamin D2 (ergocalciferol) and Vitamin D3 (cholecalciferol) which are found mainly in fish-liver oils and fortified milk.
There is one other thing you need to be aware of if you choose to use an oral vitamin D supplement and that is that there are basically two types – one is natural and one is synthetic.
Vitamin D obtained from sun exposure, food, and supplements is biologically inert and must undergo two biochemical changes (hydroxylations) in your body before it can use it. The first conversion occurs in the liver and this is one reason why animal livers are good to eat, they contain the fat soluble vitamins. Vitamin D gets converted in the liver to 25-hydroxyvitamin D [25(OH)D], also known as calcidiol. The second conversion occurs primarily in the kidney (a good reason to eat kidneys) and forms the physiologically active 1,25-dihydroxyvitamin D [1,25(OH)2D], also known as calcitriol. With regards to the sun, ultraviolet B sunlight in the range of 290-300nm is needed to convert 7-dehydrocholesterol found in your skin cells into cholecalciferol, which is the preliminary form of vitamin D3.
If your doctor or specialist has prescribed you Vitamin D, make sure it is Vitamin D3 and NOT Vitamin D2. Be aware that most prescription-based Vitamin D supplements contain synthetic Vitamin D2, so if you receive a prescription for vitamin D from your doctor, you’re most likely receiving the inferior vitamin D2.
Most of us don’t really have an issue with a lack of sun exposure in the summer months in New Zealand, but we are continually bombarded with messages of covering up from the sun inn case we develop skin cancer such as melanoma. I’m sure that those in the most northerly parts of the world can relate to plenty of sunshine in summer but a major lack of the same in the winter months.
By just spending time time outside in the summer months, you will get sufficient Vitamin D. Did you know that your body can produce about 20,000 IU of vitamin D per day with full body exposure, about 5,000 IU with 50 percent of your body exposed. But you don’t need to have that much of your body exposed, by just having as much as 10 percent of your body exposed you will get a 1,000 IU dose.
If you live in Canada, the Midwest U.S, Northern Europe, Scotland and in New Zealand you will receive low to infrequent amounts of sunshine and it is therefore critical that you monitor your levels of Vitamin D regularly. The interesting point I’d like to make is these areas are also the hotspots for many cancers and multiple sclerosis, both conditions linked strongly to Vitamin D deficiencies.
1. – Get a Vitamin D blood test done. Daily supplementation with vitamin D in the range of 1,000 – 2,000 IU may provide important health benefits for many individuals. If you do not eat a diet rich in Vitamin D, you may want to target the higher side of this range (while also increasing your intake of D-rich foods). If your diet already includes ample amounts of foods that are rich in vitamin D, you may want to target the lower side of this range when deciding on a supplementation level.
2. – If you are at a higher risk of Vitamin D deficiency or have a special requirement (osteoporosis, heart disease, multiple sclerosis, etc) I encourage you in particular to have that blood test and determine you serum level of Vitamin D. Once you have your result back it would be good to work with your practitioner to determine your appropriate level of Vitamin D supplementation. Depending on the results of your blood test, you may very possibly need a greater level of vitamin D supplementation that is greater than the 4,000 IU Tolerable Upper Limit set by the National Academy of Sciences. Blood testing can definitely help to remove the “guesswork” factor here. You’ll be able to determine the actual level of hydroxyvitamin D in your blood and see the actual amount of increase following supplementation at whatever level you and your health-care provider determine to be appropriate. The Harvard School of Public Health (and many other public health organisations) recommending supplementation with vitamin D3 (cholecalciferol) rather than D2 (ergocalciferol).
Vitamin D is found in a narrow range of foods. Good food sources are oily fish and eggs. Other food sources include fortified foods such as margarine, breakfast cereals and powdered milk. But we get most of our vitamin D from sunlight on our skin. This is because the vitamin forms under the skin in reaction to sunlight. Vitamin D is a fat-soluble vitamin which essentially means that you don’t need it every day because any of the vitamin your body does not need immediately is stored for future use in the liver mainly. Most people get all the vitamin D they need from their diet and sun. However, if you are pregnant, breastfeeding or elderly you should take at least 10 micrograms (0.01 mg) of vitamin D each day.
 |
Salmon | 100 grams | 411 iu |
| Prawns (shrimp) | 100 grams | 162.39 iu | |
| Sardines | 1 can (80 grams) | 250.24 iu | |
| Cow’s milk (2%) | 1 cup (250ml) | 97.60 iu | |
| Cod (baked, steamed) | 100 grams | 63.50 iu | |
| Egg (whole, boiled) | 1 egg | 22.88 iu |
Vitamin D has other roles in the body, including modulation of cell growth, neuro-muscular and immune function, and reduction of inflammation. Here are the most important roles that Vitamin D plays in the body.
 |
Clinical Application of Vitamin D
|
WARNING: There is no way to know if the below recommendations are correct. The ONLY way to know is to test your blood. You might need 4-5 times the amount recommended above. Ideally your blood level of 25 OH D should be 60ng/ml. However, it is important to realise that vitamin D requirements are highly individual, as your vitamin D status is dependent on numerous factors, such as the colour of your skin, your location, and how much sunshine you’re exposed to on a regular basis. If you live in New Zealand like I do (or in Scotland, Canada, North America or Northern Europe) you will have to keep a closer eye of your Vitamin D levels due to the decreasing amount of sunlight you receive, particularly in winter.
The correct blood test is 25(OH)D, also called the 25-hydroxyvitamin D blood test. It is important to have your Vitamin D test twice per year to maintain optimal health, especially as you age and become older than 50. Please note the difference between normal and optimal, you really don’t want to be average here; you want to be ideally in the optimal range.
People who lived long ago spent more time outdoors and exposed to the sun. Primitive man likely developed a tolerance to having a large exposure to UV-B and its secondary consequence to skin exposure, vitamin D.Today we obtain very little sunlight compared to long ago, and our rates of chronic disease have soared in spite of the latest science and best medical care.
Some experts may disagree with the following healthy ranges*, but they are a cross section of values taken from healthy people in parts of the world where more sunshine is experienced – the tropic and sub tropic regions. It makes sense to assume that these values are a reasonable indication of optimal human Vitamin D requirements.
* (Holick MF. Calcium and Vitamin D. Diagnostics and Therapeutics. Clin Lab Med. 2000 Sep;20(3):569-90)
I recommend to most of my patients now to have their Vitamin D levels checked regularly by way of a blood test. Blood testing is the reliable way to determine how much Vitamin D a person needs whether they be a child, adult or the elderly.
1. – Make Sure You Use the Correct Test – the 25-hydroxyvitamin D blood test.
The correct test that you need to request is the 25(OH)D, also called 25-hydroxyvitamin D, the Vitamin D marker that is most strongly associated with overall health.
2. – Determine the level of level of Vitamin D you require.
Depending on your life stage (age) and whether you have an illness or not. Please read this page through carefully to determine your requirements. If you are older you will require more D3, if you are younger you will require less. You will also find various recommendations on this page regarding Vitamin D3 dosage.
As far as Western medicine is concerned, the “normal value” for 25-hydroxyvitamin D lab range is between 20-60 ng/ml. It is important to understand that there is a difference between the normal and the optimal values in nutrition. If you look at the table below you will this that this value tends to be on the deficient side, and is to broad to be ideal. No account is taken for those who are ill, have cancer or are at varying ages.
The Recommended Dietary Allowance (RDA) is the average daily dietary intake level that is insufficient to meet the nutrient requirements of healthy individuals in each life-stage and gender group. There is sufficient scientific evidence now to validate the importance of taking the right dosage of Vitamin D depending on your individual requirements.
It has been said that it is very much compromising your health to have a Vitamin D level below 32 ng/ml, and levels lower than 20 ng/ml are considered to be a serious indication of a Vitamin D deficiency. If you have your Vitamin D blood level consistently below 20 ng/ml you risk as many as 16 different types of cancer and auto-immune illnesses such as multiple sclerosis, rheumatoid arthritis, cardiovascular disease and several more chronic illnesses.
Vitamin D Levels25 Hydroxy D |
|||
| Deficient | Optimal | Treating Cancer and Heart Disease | In Excess |
| Less than 50 ng/ml |
50 – 70 ng/ml | 70 – 100 ng/ml | More than 100 ng/ml |
An Adequate Intake (AI), a level of intake sufficient to maintain healthy blood levels of an active form of vitamin D, has been established. In 1998, the Adequate Intake levels in USA for vitamin D for adults, in micrograms (mcg) and International Units (IUs) were:
Life-stageAges 19-50 |
Men5 mcg* or 200 IU |
Women5 mcg* or 200 IU |
| Ages 51 – 69 | 10 mcg* or 400 IU | 10 mcg* or 400 IU |
| Ages 70 + | 15 mcg* or 600 IU | 15 mcg* or 600 IU |
| *1 mcg vitamin D = 40 International Units (IU) |
Evaluation of health and disease that involve vitamin D has lead many experts to the conclusion that a desirable Vitamin D blood level when treating cancer or a chronic illness is approximately between 75 nmol/L (30 ng/mL) and 100 nmol/l (40 ng/ml). It seems that many patients I have seen have a problem maintaining a Vitamin D blood level of 75 nmol/L. The latest research has shown that optimal results can be obtained by consuming up to 8,000 ug per day of Vitamin D3, especially if you are seeking cancer treatment or prevention. If this is the goal to be achieved, then why is it so difficult for most people to achieve this? In my opinion it is fear, people are made scared by their dietitian, their women’s magazine, a doctor or by other sources of mis-information. Vitamin A is similarly seen as “dangerous” and to be avoided in anything above a 5,000iu dose per day. We now know that Vitamin D in sufficient amounts has incredible benefits particularly especially the immune system, the cardiovascular system and the musculoskeletal system.
The media have over the years often reported that vitamin D nutrition status is too low in New Zealand, and that children in New Zealand are lacking in Vitamin D and that higher Vitamin D intakes may improve measures of children’s health, but that’s where it ends. In spite of what some have said in the past, from what we know right now is that most of the population have a Vitamin D level which is too low, with some experts say that optimal amounts are closer to 1000 IU daily. My recommendations? Until more is known, it is wise not to overdo it.
Based on the most recent research, the current recommendation is 70 IU’s of Vitamin D kilo of body weight. So for a child weighing 20 kgs, the recommended average dose would be 1,400 IU’s daily, and for a 85 kg adult, the dose would be nearly 6,000 IU’s. However, it is really important to understand that vitamin D requirements are unique to the individual, as your vitamin D status is dependent on many factors like the colour of your skin, where you live and how much sun you are exposed to on a regular basis. I personally would consider this dose if I had cancer or a similar chronic illness.
The Food and Nutrition Board of the American National Research Council states that 2,000 IU/day is the safe upper limit for the general population, although others have suggested that the safe upper limit may be as high as 4,000 to 10,000 IU/day. Published cases of vitamin D toxicity all involve intakes of at least 40,000 IU/day.
My advice for you is to be careful when using oral vitamin D therapy, and to make certain that you have your blood levels checked regularly, which could be three or six monthly. Many of you may choose to ignore this warning, but I am telling you in no uncertain terms, that while vitamin D has enormous potential for improving your health, it has significant potential to worsen it, if you use it improperly.
Vitamin D is potentially toxic in high doses. Infants can be affected in particular by daily amounts higher than 1000 IU, and in children and adults, sustained daily amounts over 50,000 IU can cause weakness, anorexia, vomiting, diarrhoea and mental changes. It never ceases to amaze me how people overdose on vitamins, believing that if a little is good then a whole lot more is the way to go to get a result quicker. Because Vitamin D is a fat soluble vitamin and has a tendency to build up in your body you will need to be particularly careful, and I recommend for optimal results that you are best remain under the care of a skilled health-care professional with regards to your Vitamin D requirements.
It is interesting to not that in the USA the National Academy of Sciences made revised public health recommendations in 2010 for the increased intake of vitamin D. Did you know that in the past 15 years, more than 10,000 studies on vitamin D have been published in research journals?
1. We need much more vitamin D than we previously thought.
2. Lifestyle trends have significantly reduced our exposure to sunlight.
3. Prevalence of vitamin D deficiency in Aust & NZ is much greater than previously estimated.
4. Increased Vitamin D is required to remedy deficiency than can be obtained in a standard diet.
In studies on infants and toddlers, between 40-65% have been shown to be vitamin D insufficient with blood levels of hydroxyvitamin D below 30 ng/mL in several countries throughout the world, and in studies in the U.S., including a recent study in Massachusetts. Insufficiency has also been shown in U.S. teens, at a level of approximately 60% (once again, using the standard of 30 ng/mL or less for hydroxyvitamin D in the blood). Similar percentages have been determined for insufficiency in older individuals. Among young adults and middle-aged individuals, the prevalence of vitamin D insufficiency has been estimated to range from a minimum of about 50% to a maximum of perhaps 75% or greater.
A revolution is taking place in medicine currently in our understanding of vitamin D over the past 15 years. It is very important to note that “insufficiency” refers to a blood level of hydroxyvitamin D below 30 ng/mL, and “deficiency” signifies a blood level below 20 ng/mL. While this lower blood level has traditionally been used to diagnose vitamin D deficiency, it is no longer appears relevant for determining the amount of vitamin D needed for optimal hormonal regulation of many body processes by vitamin D. This would not only count for Vitamin D, but for all the other vitamins as well.
We also realise now that it takes higher levels of vitamin D intake to bring blood levels up to a healthy standard. For example, in situations where sunlight is limited, we know that at least 1,000 IU of vitamin D are needed to increase blood levels of vitamin D from 20ng/mL to 30 ng/mL or higher. For prevention of bone loss in those at risk for osteoporosis, we know that a minimum of 700 IU is required and that no prevention results have been demonstrated at levels of intake below 400 IU. But for conditions such as autoimmune problems like rheumatoid arthritis or multiple sclerosis, experimental supplemental doses of vitamin D range not in 100s of IUs, but in 1,000s or 10,000s of IUs.
It is very difficult to make a firm and fast public health recommendation for vitamin D that is guaranteed to meet the exact and optimal requirements of each individual, because personal health history and an individual’s exposure to sunlight play such an important role in determining each individual’s needs.
Based on studies showing the impact of supplemental D3 intake on blood levels of hydroxyvitamin D, I believe that the vast majority of adults and children will not be able to achieve optimal vitamin D status from food intake alone. Exactly how much Vitamin D3 supplementation each individual may need and the frequency of blood testing should be determined with the help of your health-care professional. Your health-care professional can help evaluate your personal health history factors and can also monitor the impact of your vitamin D supplementation.
Vitamin D References
Last Page Update 7 April 2011